Table of Contents
What is Marasmus?
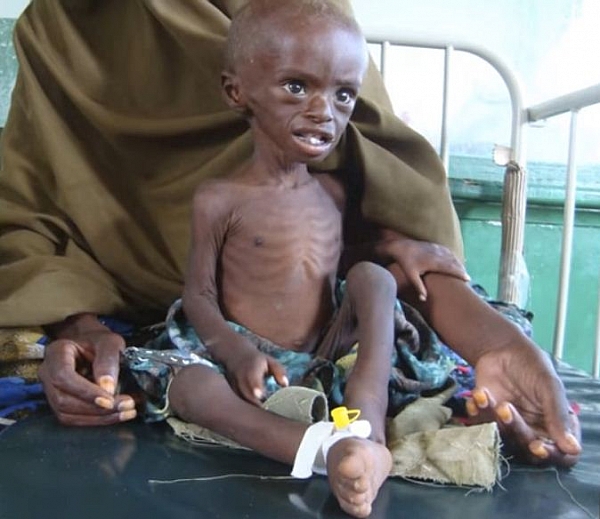
Marasmus is a form of protein-calorie malnutrition that mostly affects children, especially in developing countries because of the low standard of living. It is associated with a deficiency of both protein and energy in the diet. This is different from Kwashiorkor which results from solely protein deficiency. Marasmus is sometimes called Nutritional Marasmus because it results from an inadequate nutritional diet. It affects both adults and children but children are mostly affected as they cannot carter for themselves and rely on adults who may not provide enough of all the nutritional needs of a child.
People affected by Marasmus mostly do not have enough food to eat or the food eaten does not have the required nutrients to meet the demand of the body. Marasmus occurs commonly in children of 1 to 3 years and a half; with babies less than 1 year affected more than other age groups – breastfeeding babies are hardly affected because they get their nutrients from breast milk. This is why most cases start after a child has been weaned off breastmilk which usually occurs around 1 year.
Risk Factors and Causes of Marasmus
Inadequate diet
The failure of breastfeeding makes children less than 1 year of age to be at risk of having Marasmus. Even in children fed with express breast milk, the feeding may not be adequate for the baby and predisposes the baby. Living in areas with a high poverty rate such as developing countries is a risk factor.
Premature babies
Prematurity is a risk factor because premature babies find it difficult to suck by direct breastfeeding and thus are fed with spoons by express breast milk. The amount of breast milk needed for the premature infant to meet the demand of the body is higher than that of the normal babies; most times, the premature baby is not fed enough and is at higher risk of developing Marasmus.
Infections
Infections can cause Marasmus as they increase the demand of the body for nutrients. This usually occurs due to overconsumption of proteins and calories making the nutrients unavailable for use by the body. Diseases such as measles, diarrheal diseases, and intestinal parasites all predispose to having Marasmus.
Congenital anomalies
Congenital malformations such as the cleft palate and cleft lips make feeding difficult and leading to malnutrition. This can be complicated by infections of the respiratory tract.
Marasmus Signs and Symptoms
- Poor growth
- Muscle wasting with prominent bones and ribs
- Children with Marasmus appear miserable but are mentally alert
- Skin is usually shrunken and folded. These skin changes are not severe as Kwashiorkor
- Hair changes such as thin and brownish/red hair may occur
- Diarrhea is not common but may occur
- Intact appetite
- Wizened old man’s face (dried and shrunken facial appearance)
- Anemia
- Flattened abdomen with a big head sometimes
Poor growth
A child with Marasmus fails to grow properly, and the height and weight will be below the normal range for his/her age because of the inadequate protein and other nutrients required for normal growth.
Wasting of the muscles
The muscles are grossly wasted and the subcutaneous fats are depleted making the ribs and bones very prominent. The skin of the buttocks, the arms, and thighs are folded and dry. The eyes are sunken.
Mental alertness
The child with Marasmus is mentally alert and less miserable than Kwashiorkor but has the wizened facial appearance.
Skin and hair changes
There may be hair and skin changes in Marasmus but not as severe as in Kwashiorkor. Discoloration of the hair from black to yellow or brown. Scanty hair on the scalp.
Voracious appetite
The appetite is intact and they are often found sucking their hands or anything within their reach to find some succor. When given food, they eat voraciously.
Diarrhea
Diarrhea may occur but not common. If it occurs, dehydration may follow.
Diagnosis of Marasmus
Diagnosis is made clinically using the age and weight of the child and relating it with the criteria in the Modified Wellcome classification of malnutrition. A child is said to have Marasmus when the weight for age is less than 60% without body swelling (i.e no edema). When the weight for age is less than 60% with body swelling, then the child is said to have Marasmic-Kwashiorkor, which is a combination of the features of Marasmus and Kwashiorkor.
Laboratory investigations in the management of Marasmus
Laboratory tests are often done in order to help diagnose the presence of co-existing infections that may affect treatment; hence these tests help in treatment. These tests do not show if a child has Marasmus or not, as diagnosis depends on clinical findings and examinations.
- Packed cell volume (PCV) is used to check for the presence of anemia
- Differential white blood cell (WBC) checks for infections in the body
- Urinalysis and urine microscopy checks for infections of the urinary tract
- Stool microscopy helps in the diagnosis of intestinal parasites or occult blood in the stool
- Chest X-ray can diagnose tuberculosis, pneumonia or any chest infection
Treatment of Marasmus
The management of Marasmus involves adequate dietary therapy and treatment of factors that caused the disease as well as treating any associated condition. It is treated just like treatment for any other form of severe protein-calorie malnutrition.
Treatment phases and timelines for Marasmus
- Stabilization phase
- Rehabilitation phase
- Follow up phase
Stabilization phase
This involves stabilizing the abnormalities in electrolytes, blood glucose, body temperature, and fluids. It includes checking and treating:
- Hypoglycemia using dextrose or by initiating feeding
- Hypothermia using warm clothing and kangaroo mother care for babies.
- Dehydration using Resomal
- Electrolytes disorders and mineral deficiencies
- Any associated infection
The treatment in the stabilization phase should be carried out within the first two days of admission to prevent life-threatening conditions such as hypothermia (low body temperature), hypoglycemia (low blood glucose), infections, and dehydration.
Rehabilitation phase
This a continuation of the treatment in the stabilization phase and also involves taking a good medical history and physical examination to know the cause of the Marasmus and appropriately treating the cause with any associated medical conditions.
Follow up phase
There is a need to follow up to make sure the child is gaining appropriate weight and to minimize any long term complications.
Complications of Marasmus
- Severe infections often always occur such as Pneumonia
- Electrolyte disorders with their associated complications
- Stunting
- Low immunity that may give rise to opportunistic infections
- Coma and Death
Prevention of Marasmus
- Adequate feeding of children, especially those that have been completely weaned-off breast milk or inappropriate weaning practice. Their diet should contain all the required nutrients. Varying of food helps control nutrient deficiency.
- Use of Oral rehydration therapy for the treatment of diarrhea
- Practice Exclusive Breastfeeding and a baby should be breastfed on demand
- Proper Immunization of children to prevent infections
- Family planning should be done to ensure proper spacing of children