Table of Contents
What is Tuberous sclerosis?
Tuberous sclerosis is also called Bourneville disease or Bourneville phakomatosis or Epiloia or Pringle disease. It is a rare genetic disease that is autosomal dominant in nature which means that it can be transferred from parent to child by inheritance of a single defective gene. It is best described as a disease complex because it occurs as a result of the interaction of multiple gene mutations and environmental factors; the mode of inheritance is difficult to predict because you cannot know which of the parents can transmit the disease or who can inherit the disease because the pattern of inheritance is not clear cut, even within the same family, the severity of the disease varies greatly; what can explain this variability is the germline mosaicism in which parents who do not have a disease may have several offspring with the disease (this is mostly seen in autosomal dominant and X-linked disorders). TSC affects many organs of the body; because of these factors, it is better called Tuberous Sclerosis Complex and abbreviated as TSC. It is given the name Tuberous sclerosis because the tumors in the brain and other affected organs appear as tubers of potato.
Tuberous sclerosis is a neurocutaneous syndromebecause it affects structures or organs that arise from the neuroectoderm; it sometimes affects the organs originating from the endoderm as well as mesoderm.
Structures arising from the Neuroectoderm that are affected in Tuberous sclerosis:
- Brain and spinal cord
- Skin
- Bones of the head
- Connective tissues of the head and face
- Some parts of the peripheral nervous system
Tuberous sclerosis can cause tumors of the above-listed organs such as the skin, spinal cord, brain, and bones.
This disease can be managed to help relieve some of the symptoms but cannot be cured, this means it has to be managed for as long as the individual lives.
Epidemiology
Tuberous sclerosis complex affects 1 in 6800 – 15,000 births. It is among the common causes of infantile spasms. There is great variability among those affected with the abnormal genes as some individuals have mild symptoms while others have severe symptoms i.e. there is great variability in the disease penetrance.
70% of TSC cases have no history of the disease in their family and therefore occurs sporadically, pointing to the fact that the genetic mutation might have occurred after birth. If the genetic mutation occurs sporadically, the gene affected is mostly the TSC2 than the TSC1 gene. It has been observed that mutations affecting the TSC1 gene give rise to the milder forms of the disease.
Pathogenesis of tuberous sclerosis
There are genes in the body that function to suppress tumors from occurring, these set of genes are called tumor suppressor genes. When there is a genetic change (mutation) in these suppressor genes to an extent that their function is inactivated, then tumors can form; the two of these suppressor genes have been implicated in causing tuberous sclerosis complex, they are the TSC1 and TSC2 genes located on chromosome 9 and 16 respectively. These genes serve as templates for making the proteins necessary for suppressing tumor growth in the body. TSC1 gene encodes a protein called hamartin while theTSC2 gene encodes for the tuberin protein. These two tumor suppressor proteins form a complex that limits the activity of an enzyme called mTOR (mechanistic target of rapamycin) kinase; without suppression, mTOR kinase activity leads to increased protein synthesis as well as increase in cell size which then lead to abnormal growth of cells causing the tumors seen in different organs of the body in tuberous sclerosis complex.
According to the model of how tumor suppressor gene works, for TSC1 or TSC2 gene to become inactive, there must be two successive mutations affecting either the TSC1 gene or TSC2 gene. The first mutation is usually inherited but a single mutation cannot make the genes not to work properly; hence a second mutation is needed to cause inactivation of the gene before the cell can start multiplying to form tumors. This second mutation occurs after fertilization and is required to induce tumor transformation. Transmission of Tuberous sclerosis beyond two generations is rare as a result of a reduction in fertility of individuals affected by this disease.
Genetic studies on TSC were done using the Eker rat as an animal model.
Symptoms and Signs of Tuberous Sclerosis Complex
The common finding in TSC is the presence of Hamartomas which are normal tissues in appearance but their rate of growth is rapid and they can be found in abnormal sites.
What is the classic triad of TSC?
- Seizures
- Mental retardation
- Facial angiofibroma (adenoma sebaceum)
But not all patients with TSC manifest these classic features.
What is the most common presenting symptom of TSC?
The commonest presenting symptom is seizures. This occurs in about 85% of patients including children who present with epileptic spasms (or infantile spasms).
Central Nervous System features
- Presence of cysts and sclerosis in the cortex of the brain
- Brain tumors – gliomas along the lateral walls of the lateral ventricles occur in 80% of cases
- There could be calcification of the basal ganglia
- Neonatal seizures in newborns of age 2 to 4 weeks
- Repeated seizures (Epilepsy) in over 90% of cases of TSC
- Mental retardation in 50% of cases
- Autism
Retina
There are two types of hamartomas seen in the retina; one is large and nodular, often found at the optic disc area while the other is found in the posterior pole and is greyish white in color with a soft consistency.
Skin features
The clinical manifestations of tuberous sclerosis complex on the skin in affected individuals above the age of 5 years include:
- facial angiofibromas or adenoma sebaceum these often appear at puberty as pink or yellowish acne-like papules on the face, especially around the nose. They are distributed in a butterfly pattern over the cheeks, chin, and forehead
- hypo-pigmented macules (or the ash leaf macules) these are small white oval patches that occur in over 90% of cases that could be the only finding at birth (to be significant, they should be three or more)
- Ungual fibromas (Koenen tumors) these occur in 15% of cases and mostly develop in adult life. They are small sausage-like in appearance and pink in color and found under nail folds in the absence of any trauma to the affected nails.
- Connective tissue naevi (shagreen patches) these are seen in 50% of cases and they appear like cobblestone but somewhat yellow in color and mostly arise from the skin over the base of the spine. They mostly occur at the lumbar and gluteal regions; they appear in late childhood or early adolescence
- Caf-au-lait spots in about 25% of cases and mostly appear at puberty.
Other dermatologic findings include pitting of dental enamel and facial skin hamartomas on cheek, chin and dry site of skin. There could be gingival fibromas that can be exacerbated when taking antiepileptic drugs (thereby causing drug-induced gingival hyperplasia).
Skin findings in tuberous sclerosis according to the age of onset
AGE AT ONSET |
SKIN FINDINGS |
INCIDENCE (%) |
Birth or Later |
Hypopigmented macules |
80 |
2-5 yr |
Angiofibromas |
70 |
2-5 yr |
Shagreen patches |
35 |
Puberty |
Periungual and gingival fibromas |
20-50 |
Birth or Later |
Caf-au-lait spots |
25 |
Renal Findings
The kidney is most often affected with various manifestations as listed below:
- Renal angiomyolipomas most of the kidney lesions are angiomyolipomas, as much as 85% of cases
- Renal cysts occur in 30 to 47% of cases
- Renal cell carcinoma occurs in 2-3% of TSC cases affecting the kidneys
- Other less common renal findings include
- Interstitial fibrosis with focal segmental glomerulosclerosis (FSGS)
- Glomerular microhamartomas
- Peripelvic and perirenal lymphangiomatous cysts
The rate of progress of renal features is slow but is the most common cause of death in patients with tuberous sclerosis complex. Most times, death occurs as a result of retroperitoneal bleeding or renal failure.
Renal Angiomyolipomas
Renal angiomyolipomas are abnormal blood vessels growing in the kidneys; these lesions could be solitary or diffuse; the walls of these vessels are thick and made up of fat tissues and smooth muscle-like cells. Even though these lesions are benign, they can locally invade into the perirenal fat and in rare instances could extend into the renal vein and even the inferior vena cava and right atrium. The invasion of angiomyolipomas causes renal symptoms such as retroperitoneal hemorrhage, tenderness in the flanks, hypertension, and impairment of renal function. On examination, the masses can be felt in flanks.
The solitary angiomyolipomas can be seen even in people without TSC especially in elderly women but these type can be distinguished from those occurring as result of TSC because TSC related angiomyolipomas are usually bilateral (affects both kidneys) and multiple; they mostly occur after 5 years of age and increase in number and size as the age increases.
These lesions are larger in women than men and there is an increased risk of bleeding and rupture in pregnant women.
Renal Cystic Disease
Renal cysts can occur as early as infancy starting mostly in the renal cortex but can occur also in the glomerulus and then increase in number and size as the age of the patient increases. Histologically, the cells lining the epithelia of these renal cysts in TSC are unique, the cells with hyperchromatic nuclei and sometimes mitotic figures are seen. Associated with these cysts are adenomas and hyperplasia of the papillae.
A small number of children less than 1 year of age could have massive renal cystic disease with severe hypertension and progressive renal impairment that leads to end-stage renal disease in the second or third decade of life. This happens because there is a deletion in the TSC2 and PKD1 genes causing the PKDTS contiguous gene syndrome (Polycystic Kidney Disease). The life span of patients with PKDTS contiguous gene syndrome can be increased by early recognition of this syndrome and prompt control of infantile spasms and strict blood pressure control.
There could also be cysts in the liver and pancreas.
Renal Neoplasms
There are common multifocal benign epithelial tumors associated with tuberous sclerosis complex such as oncocytomas and papillary adenomas but in rare instances, renal cell carcinomas could occur with a 2% to 3% lifetime risk of developing RCC.
These renal cell carcinomas have unique clinical features and pathogenesis. They occur mostly in females than males and are mostly diagnosed in younger age groups and are found associated with angiomyolipomas. The renal cell carcinomas progress slowly and multiple in number. There are 3 histologic types of renal cell carcinoma associated with TSC and they include the common papillary cell carcinoma, followed by hybrid oncocytic/chromophobe tumor and the less common type of renal cell carcinoma with granular eosinophilic morphology.
Skeletal system
The unique finding in the skeletal system is punctate osteosclerosis. These lesions may be round, oval, or irregular in outline, and they may vary in size from a few millimeters to several centimeters. Sclerosis can also occur in the ribs and spine. Periosteal new bone formation along the shafts of the large and small tubular bones may be seen. Small, cyst-like lesions occur in the small bones of the hands and feet.
Cardiopulmonary
- Pulmonary lymphangioleiomyomatosis these are a rare abnormal proliferation of smooth muscle cells occurring in the lungs, pleurae, lymphatics and blood vessels. They occur only in women of younger age group and give rise to symptoms such as difficulty in breathing, coughing of blood, spontaneous pneumothorax and chest pain.
- In the heart there are cardiac rhabdomyomas that can cause arrhythmias or cardiac outflow obstruction
Diagnostic criteria for Tuberous sclerosis complex
The diagnosis of tuberous sclerosis complex is based on the diagnostic criteria made by the National Institutes of Health Consensus Conference in 1998. These diagnostic criteria include major and minor features.
How to use the major and minor criteria
- A definite diagnosis of TSC is made when there are two major features or when there is one major feature with two minor features
- A probable diagnosis of TSC is made when there is one major feature and one minor feature
- A possible diagnosis of TSC is made when there is only one major feature only or when there are two minor features without a major feature
The major features of Tuberous sclerosis complex
- Facial angiofibromas or forehead plaque
- Nontraumatic ungual or periungual fibroma
- Presence of more than three Hypomelanotic macules
- Shagreen patch or connective tissue nevus
- Multiple retinal nodular hamartomas
- Cortical tuber(s)
- Subependymal nodule
- Subependymal giant cell astrocytoma
- Presence of a single Cardiac rhabdomyoma or more
- Lymphangioleiomyomatosis
- Renal angiomyolipoma
The minor features of TSC
- Multiple and random dental pits
- Hamartomatous gastrointestinal or rectal polyps
- Bone cysts
- White matter radial migration lines
- Gingival fibromas
- Non-renal hamartoma
- Retinal achromic patch
- Confetti skin lesions which are clusters of low melanin lesions with a reticular appearance
- Multiple renal cysts
The features of tuberous sclerosis complex are found on the physical examination of patients, the use of various kinds of imaging techniques and biopsy. Not only does imaging help in diagnosis but also in monitoring the progress of the disease. Some of the imaging techniques and the features they detect are discussed below.
Renal diagnostic modalities
Renal imaging is mostly for monitoring disease progression in patients with TSC as the cause of death is mostly due to renal failure.
Ultrasound has been the modality of choice over the years and is highly sensitive in the detection of renal cysts and in angiomyolipomas that are rich in fats but poor in detecting renal lesions with low fats.
The use of abdominal CT or magnetic resonance imaging (MRI) is recommended every 1 to 3 years for monitoring the progression of angiomyolipomas and renal cysts.
Sometimes a renal biopsy is needed to distinguish between a renal angiomyolipoma and renal cell carcinoma.
Other diagnostic modalities
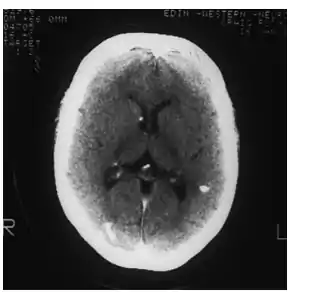
- Computed tomographic scans and MRI help to detect calcifications of subependymal nodules or dysmyelinating white matter lesions.
- Cardiopulmonary lesions can be detected using chest X-ray and Echocardiography
- Ophthalmoscope (Funduscope) is used in viewing retinal hamartomas
Management of tuberous sclerosis complex
- Use of Vigabatrin in the symptomatic treatment of seizures this drug is very effective in the management of infantile spasms in TSC. The drugworks by binding to the degradative enzyme GABA transaminase receptor thereby causing an increase in GABA levels and inhibition of neurotransmission. Vigabatrin is also useful as adjunctive therapy for poorly controlled seizures and has a plasma half-life of 58 hours. However, it has the side effect of causing visual field constrictions and also causes a reduction in level plasma phenobarbital and phenytoin levels. Vigabatrin comes as 500mg tablets and 500mg sachets.
- When medical management fails to control seizures, surgical resection of cortical tubers (which are often epileptogenic) may be beneficial
- Renal Angiomyolipomas: in most cases, they are benign and require no treatment; but sometimes may become very large and form aneurysms with the attendant risk of bleeding especially at diameters of more than 5cm. When there is a risk of bleeding, treatment is usually through nephron-sparing surgery or embolization.
- If there is a suspicion of renal cell carcinoma in the presence of increased cell sizes with accompanying pain or bleeding, then nephron-sparing surgery, such as enucleation or partial nephrectomy is carried out.
- Women with angiomyolipomas should be advised not to get pregnant and should avoid the use of estrogen pills because of the increase in size and number of angiomyolipomas with an associated risk of hemorrhage noticed during pregnancy. This shows that female sex hormones are capable of accelerating the growth of Angiomyolipomas.
- Since TSC arises following a defective mTORC1 signaling, the use of mTOR inhibitors (rapalogs) is recommended in the first-line treatment of asymptomatic and growing angiomyolipomas that are larger than 3cm.
- Sirolimus and everolimus are useful in reducing the volume of angiomyolipomas even though they have their adverse effects.
- Renal cystic disease is mainly treated by strict BP control. Though some doctors try surgical decompression of cystic kidneys, there has been no significant benefits.
- In patients with TSC and chronic kidney disease, renal replacement therapy is beneficial. This includes dialysis and renal transplant. It is advisable to have bilateral nephrectomy before initiation of renal replacement therapy because of the risk of renal hemorrhage and malignant transformation associated with angiomyolipomas.
- Cosmetics can be achieved in TSC facial angiofibromas by use of electrodesiccation, dermabrasion or destruction of lesions by laser; even though these lesions tend to recur.
- Genetic counseling – affected families need genetic counseling especially in parents who do not have the disease but have a child who has the disease. Such parents may wish to know the chances of further children being affected. It is good to examine the parents of an affected child to know if it is from a new mutation or from parents. This can be done using Woods UV light; there is also a need for the parents to be examined by an ophthalmologist to help exclude the possibility of genetic transmission from a subtly affected parent. Genetic testing of family members is also advised.
Differential diagnosis of TSC
- The differential diagnosis for ash leaf macules includes vitiligo and naevus anaemicus.
- The adenoma sebaceum lesions may look like acne.
- Hypomelanosis of Ito
- Sturge-Weber syndrome
- Birt-Hogg-Dube syndrome
- MEN (multiple endocrine neoplasias)
Complications that may occur in a child with Tuberous sclerosis
- The child may have seizures (Epilepsy)
- There may be associated Autism
- Enlarged Kidneys because of bilateral renal cysts
- Increase risk of renal malignancy
- Mental retardation
- Pneumothorax can develop
- Obstruction of cerebrospinal fluid outflow and resultant hydrocephalus caused by subependymal nodules that may mutate into subependymal giant cell astrocytomas that cause the blockage.
TSC Prognosis
There is poor prognosis in the presence of severe epilepsy and mental retardation as most do not live beyond 30 years of age because death usually results from repeated seizures, associated neoplasms or intercurrent illness.