Table of Contents
What are gram positive bacteria?
Gram positive bacteria are those examples of bacterial cells with a thicker peptidoglycan structure in their cell wall. In bacteriology, gram-positive bacteria can be defined as the bacteria that stain blue/purple, giving a positive result in a gram stain test. These bacteria are different from the gram-negative bacteria that have a thin peptidoglycan cell wall and stain red to pink in the gram stain test. A gram stain test is a differential staining technique that is used to differentiate bacterial cells into gram-positive or gram-negative cells.
The most common gram-positive bacteria examples in microbiology include Staphylococcus, Streptococcus, Bacillus, Clostridia, Listeria, and Corynebacterium. These gram-positive bacteria representative species are pathogenic and cause several diseases. All gram-positive bacterial cells are bounded by a single-unit lipid membrane. Generally, the cell walls of gram positive bacteria contain a 20-80 nm thick layer of peptidoglycan. This peptidoglycan is the molecule responsible for retaining the gram stain.
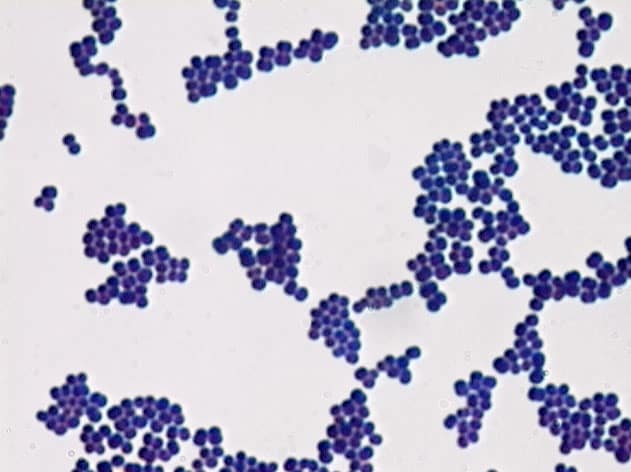
Photo credit: www.atsu.edu
Gram positive bacteria have a thick layer of peptidoglycan in their cell wall compared to gram-negative bacterial cells. The peptidoglycan layer of the gram-negative cell wall is 2-3 nm thick and covered with an outer lipid bilayer membrane whereas the gram-positive cell wall is a 20-80 nm thick polymer. Nevertheless, despite gram-positive bacteria having a thicker peptidoglycan layer, they are more receptive to certain cell walls targeting antibiotics than gram-negative bacteria. This is due to the absence of the outer membrane in the gram-positive cell.
Furthermore, there are other bacterial cells that are bounded by a single membrane as the gram-positive bacteria but stain gram-negative due to the lack of the peptidoglycan layer e.g Mycoplasma or their inability to retain the gram stain due to the composition of their cell wall. Bacterial cells that are bounded by a single cell membrane are called monoderms whereas, those bounded by an inner and outer cell membrane are called diderms .
Gram stain test and its use in classification of bacteria
According to the gram stain test, bacteria are traditionally divided into two groups:- gram-positive and gram-negative. This classification is ambiguous though because it is based on three distinct characteristics which include staining results, envelope organization, and taxonomic group. Classification with these three aspects does not necessarily work for some bacterial species.
The gram staining response of bacterial cells is an empirical criterion. This differential staining technique is based on the distinct differences in the ultrastructure and chemical composition of the bacterial cell wall, which is due to the presence or absence of an outer lipid membrane. Gram staining involves 4 steps which include the application of a primary stain (crystal violet), the addition of a mordant -iodine), decolorizing with alcohol, and counterstaining.
During the gram stain procedure, bacteria that are gram-positive take up the crystal stain used in the test. Thus, the stained gram positive bacteria appear purple/ blue under the microscope. This is attributed to the cell wall structure of the bacteria. The cell walls of gram positive bacteria contain thick peptidoglycan layers that retain the primary stain of the crystal violet used even after the decolorization stage of the gram staining steps. Therefore, after the gram stain procedure, gram positive bacteria stain purple or blue.
The gram-negative bacteria, on the other hand, are unable to retain the violet stain after decolorizing because the alcohol used in the decolorization step degrades the outer membrane of the cells. This makes the cell wall more porous and unable to retain the crystal violet stain. The peptidoglycan layer of the gram-negative cell is much thinner and incorporated between an inner cell membrane and a bacterial outer membrane. This is why they take up the counterstain (safranin or fuchsine) color and appear red or pink compared to the purple or blue color of gram-positive bacteria.
Gram positive bacteria characteristics
- One of the characteristics of gram positive bacteria is the presence of a cytoplasmic lipid membrane which is surrounded by a cell wall.
- The cell walls of gram positive bacteria contain peptidoglycan, polysaccharides, teichoic acids, and proteins.
- When viewed under a microscope, gram positive bacteria appear purple after a gram stain test.
- These bacteria have a much smaller volume of periplasm than that in gram-negative bacteria.
- The presence of a thick peptidoglycan layer is one of the distinct characteristics of gram positive bacteria.
- They have teichoic acids and lipoids that form lipoteichoic acids in the cell wall. This lipoteichoic acid serves as a chelating agent, and also function for certain types of adherence.
- Some species have certain surface appendages such as flagella, which help them move.
- The gram positive bacteria without flagella have two basal body rings that support them.
- Another common gram positive bacteria characteristics are the crosslinking of peptidoglycan chains by a bacterial enzyme DD-transpeptidase to form rigid cell walls.
- Some gram positive bacterial species have a capsule that consist of polysaccharides.
- They have an S-layer that is attached to the peptidoglycan layer.
- They do not have an outer membrane as gram negative bacteria does.
- The cell wall structure of gram positive bacteria is complex and can easily absorb foreign material.
- These bacterial cells rarely have hair-like structures called pili. However, pili can be seen in some gram positive species like Streptococcus and Corynebacterium.
Gram positive bacteria structure
There are two main features that differ the structure of gram positive bacteria from gram-negative bacteria. These features include the thickness of the peptidoglycan layer and the presence or absence of the outer lipid membrane. This is because it is the cell wall structure that affects the ability of the bacterial cell to retain the crystal violet stain used in the Gram staining procedure.
Cell envelope of gram positive bacteria
The cell envelope of gram positive bacteria consists of two to three layers which include the cytoplasmic membrane, cell wall, and in some, an outer capsule.
Capsule
A capsule is a third protective covering in some species of gram-positive bacteria. This covering is made up of polysaccharides (complex carbohydrates). The function of the capsule is to prevent the bacterium from drying out. This gram-positive bacteria structure also protects the bacterial cell from being engulfed by larger microorganisms. Streptococcus pneumoniae is one of the common pathogenic gram-positive bacteria examples that possess the capsule. This capsule is a major virulence factor in these disease-causing bacteria. However, the nonencapsulated mutants of such bacteria are avirulent, thus, they don’t cause disease.
Cytoplasmic membrane
The cytoplasmic membrane is a layer structure of gram positive bacteria that consists of phospholipids and proteins. This membrane encloses the interior of the bacterial cell. It also regulates the inflow and outflow of materials in the cell. This structural trait is a common trait of bacteria with all other living cells. It is a barrier that permits the cells to selectively interact with their environment.
Gram positive bacteria cell wall
The cell walls of gram-positive bacteria contain peptidoglycan, lipid, teichuronic acid, and teichoic acid. This structural component is different from the gram-negative bacteria cell wall that is made up of peptidoglycan, and the outer membrane (that consists of lipid, protein, and lipopolysaccharides). The gram positive bacteria cell wall is therefore thick and takes up the crystal violet dye of the gram stain. Hence, the gram positive bacteria under the microscope appear purple.
The main component of the cell wall structure of gram positive bacteria is the peptidoglycan layer which makes up 95% of the cell wall. Peptidoglycan contains a polysaccharide structure that has an equal amount of alternating N-Acetylmuramic acid (NAM) and N-acetylglucosamine (NAG) residues. In the cell wall structure of gram positive bacteria, the matrix substance may be polysaccharides or teichoic acids.
The teichoic acids are only found in gram-positive bacteria. They are anionic polymers made of polyglycerol phosphate units (approximately 20–30 repeats). Teichoic acid in gram positive bacteria is of two main polymer types which include ribitol teichoic acids and glycerol teichoic acids. These acids are involved in the regulation of the morphology and division of the cell. Teichoic acids can represent up to 50% of the dry weight of the gram-positive bacteria cell wall.
The gram positive bacteria cell wall can be dissolved completely by lysozymes. This lysozyme enzyme attacks the bonds between N-acetylmuramic acid and N-acetylglucosamine. However, some gram positive bacteria representative species such as Staphylococcus aureus are resistant to lysozymes. This is because these bacterial species have O-acetyl groups on carbon-6 of some muramic acid residues.
Cytoplasm
This gram positive bacteria structure is a gel-like matrix that contains other cell structures such as ribosomes, a chromosome, and plasmids. The cytoplasm is made up of water, nutrients, enzymes, gases, and wastes. This matrix of the bacterial cell is where the growth, metabolism, and replication of the cell is carried out.
The cytoplasm and its components are enclosed in the cell envelope. Since bacteria do not have a membrane-enclosed nucleus, the chromosome (a single, continuous strand of DNA) is located in the nucleoid of the cytoplasm. Whereas, all other cellular components are scattered throughout the cytoplasm.
Plasmids
The plasmids are small extrachromosomal genetic structures of many strains of bacterial cells. Similar to the chromosome, they are made of a circular piece of DNA. However, they are not involved in reproduction like the chromosome. It is only the chromosome that has the genetic instructions responsible for starting and carrying out cell division or binary fission.
Independently of the chromosome, plasmids replicate, and even though they are not essential for survival, they tend to give bacteria a selective advantage. There are two means by which plasmids are passed on to other bacteria. One means is during binary fission, whereby copies of the plasmids in the cytoplasm are passed on to daughter cells. The other means is during conjugation, a process whereby bacteria exchange genetic information. During conjugation, copies of the plasmids are passed to other bacteria by a tubelike structure called a pilus.
Plasmids have been seen to be an instrument in the transmission of special properties, like resistance to heavy metals, antibiotic drug resistance, and virulence factors essential for the infection host organisms. In the fields of molecular biology and genetics, the ability to insert specific genes into plasmids has made them extremely useful tools in genetic engineering.
Nucleoid
The region of the cytoplasm where the chromosomal DNA is located is called the nucleoid. This is not a membrane-bound nucleus. It is just an area of the cytoplasm where the strands of DNA are localized. The majority of bacteria have a single, circular chromosome for replication, while few species have two or more.
In a DNA or RNA molecule, there is a percentage of nitrogenous bases that are either guanine (G) or cytosine (C) called the guanine-cytosine content (GC-content). According to the GC-content, we have two types of gram positive bacteria which include the high g c gram positive bacteria and low g c gram positive bacteria. The DNA with low GC content is less stable than the high GC content DNA.
High g c gram positive bacteria
These bacteria have a high (≥60%) proportion of guanine and cytosine nucleotides in their chromosomal DNA. They are commonly referred to as the high g+c gram positive bacteria. A typical example is the Actinobacteria group. These bacteria have lifestyles that vary from saprophytic to obligately pathogenic.
This group of gram-positive bacteria includes gastrointestinal tract (GIT) inhabitants ( Bifidobacterium spp.), soil inhabitants ( Streptomyces spp.), pathogenic strains (e.g. Mycobacterium spp., Nocardia spp., Tropheryma spp.), and plant commensals ( Leifsonia spp.). The vast majority of the actinobacteria group are aerobic gram-positive bacteria.
Low g c gram positive bacteria
These bacteria have less than 50% proportion of guanine and cytosine in their DNA. This bacterial group includes a lot of pathogenic genera of bacteria. Clostridia is one large and diverse class of low g+c gram positive bacteria.
Clostridium, a rod-shaped bacteria are the best-studied genus of this class. These bacteria are generally obligate anaerobes that produce endospores that may survive for many years. Clostridium is found in anaerobic habitats such as soil and aquatic sediments rich in organic nutrients. Other examples of gram positive bacteria with low g c content DNA include Lactobacillus, Leuconostoc, Enterococcus, and Streptococcus.
Flagella
Flagella are whiplike structures that provide a means of movement for the bacteria that possess them. This structure beats in a propeller-like motion to help the bacterium move. The bacterium may move away from toxic chemicals, move toward nutrients, or towards the light, if photosynthetic.
Ribosomes
Ribosomes are microscopic “factories” in bacterial cells. Bacterial ribosomes translate the genetic code from the molecular language of nucleic acid to that of amino acids. This amino acid is the building block of the proteins that perform all the functions of cells and living organisms. The ribosomes in bacterial cells are smaller than those in eukaryotes and have a slightly different composition and molecular structure. These ribosomes are not bound to other organelles as in eukaryotes, rather they are free-standing structures distributed throughout the bacterial cytoplasm.
Gram positive bacteria diagram

Photo credit: www.open.oregonstate.education
Classification
Gram staining is a differential technique used to differentiate bacterial cells. Hence, these bacterial cells are classified according to the gram staining test result along with the cell shape. Moreso, the subdivision and classification of gram-positive bacteria are based on gram staining tests, as well as growth requirements, antibiotic susceptibility testing, and other macroscopic and physiologic tests.
Types of gram positive bacteria
- Gram positive cocci
- Gram positive bacilli
Gram-positive bacteria are further divided into two types based on the cell shape:
Gram positive cocci
This type of gram-positive bacteria is oval or circular in shape. Cocci mean sphere and indicate that generally, the bacteria are round. This group includes two kinds of bacteria, Staphylococcus (catalase-positive), which grows in clusters, and Streptococcus (catalase-negative), which grows in chains. Streptococcus bacteria grow in chains because their cells don’t separate completely after division.
Staphylococcus can exist on the skin and mucous membranes of humans without causing problems. However, they tend to cause serious infections when they enter the body. Streptococci also exist in the body and can be found in the skin, mouth, intestinal tract, and genital tract of humans. Nowadays, it has been discovered that septic shock due to gram positive bacteria is caused by gram-positive cocci that are aerobic. This group of bacteria is now the most common cause of septic shock and sepsis due to either direct infection, toxin production, or even both.
The staphylococci are then further subdivided into coagulase-positive (S. aureus) and coagulase-negative (S. epidermidis and S. saprophyticus) species. Whereas, Streptococci are further subdivided into Strep. pyogenes (Group A), Strep. agalactiae (Group B), enterococci (Group D), Strep viridans, and Strep pneumonia.
Gram positive bacilli
This type of gram-positive bacteria is shaped like rods. They are mostly found on the skin flora though some can cause severe medical conditions. This group of bacteria is further classified into the following based on their ability to produce spores:
- Spore-forming: When conditions are unfavorable some gram positive bacteria form spores to survive conditions like deficiency of nutrients, exposure to chemicals, or radiation. These bacteria that form spores include gram positive bacteria such as Bacillus and Clostridia. The ability to form spores makes these bacteria survive harsh conditions, making them resistant to heat, toxins, radiation, and dryness. These spore-forming bacilli can be subdivided based on their oxygen need. Bacillus are aerobic and require oxygen while Clostridia are anaerobic and don’t require oxygen.
- Non-spore-forming: These bacteria don’t form spores and include gram positive bacteria such as Listeria and Corynebacterium species. Corynebacterium are aerobic and require oxygen while Listeria bacteria are anaerobic and don’t require oxygen.
Classification of gram positive bacteria flow chart
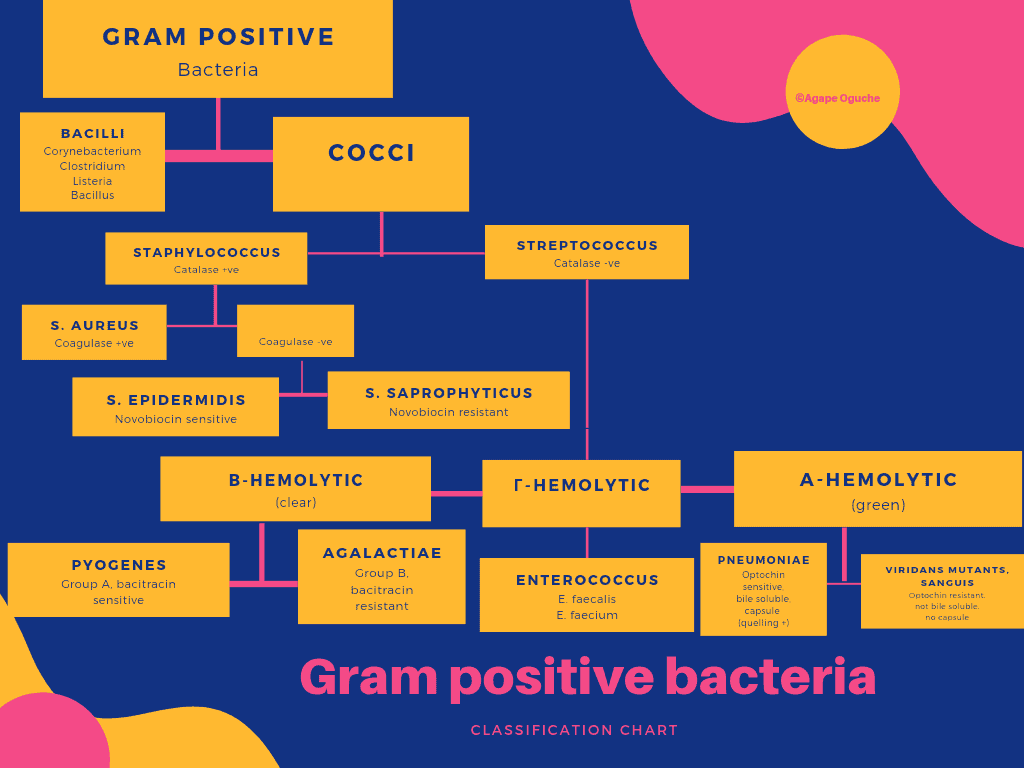
List of gram positive bacteria examples
- Micrococcus
- Enterococci
- Staphylococcus aureus
- Staphylococcus epidermidis
- Staphylococcus saprophyticus
- Streptococcus pneumoniae
- Streptococcus viridans
- Streptococcus pyogenes
- Streptococcus agalactiae
- Clostridium tetani
- Clostridium botulinum
- Clostridium perfringens
- Clostridium difficile
- Bacillus anthracis
- Corynebacterium diphtheria
- Listeria monocytogenes
The above gram positive bacteria list are the common representative species
Micrococcus
This is a genus of bacteria that belong to the Micrococcaceae family. They inhabit a wide range of environments including soil, water, and dust. These bacteria are examples of gram-positive bacteria (cocci) and range from 0.5-3 micrometers in diameter. Micrococcus normally appears in tetrads.
These organisms are opportunistic pathogens even though they are thought to be saprotrophic or commensal (see commensalism) organisms. They particularly choose hosts with compromised immune systems such as HIV patients. Because micrococcus is normally part of the skin microflora, it can be difficult to identify them as a cause of an infection. Hence, the genus is rarely linked to disease.
However, there are rare cases where immunocompromised patients die as a result of pulmonary infections caused by this genus. Also, they may be involved in other infections such as cavitating pneumonia (immunosuppressed patients), septic arthritis, recurrent bacteremia, meningitis, septic shock, and endocarditis.
Enterococci
Another example of gram-positive bacteria is Enterococcus, a large genus of lactic acid bacteria. This genus is a gram-positive group D cocci, usually seen in the colonic flora. These organisms usually occur in pairs (diplococci) or short chains. Hence, if judging by physical appearance alone, Enterococci are difficult to distinguish from streptococci. Enterococcus faecalis and Enterococcus faecium are the two common species of the genus that are commensal organisms in the intestines of humans.
Furthermore, Enterococci are among the pathogenic gram-positive bacteria as they are known to cause clinical infections such as UTIs (urinary tract infection), biliary tract infections, bacterial endocarditis, spontaneous bacterial peritonitis, diverticulitis, meningitis, and bacteremia. Nevertheless, antibiotics such as ampicillin, penicillin, and vancomycin can be used to treat sensitive strains of these bacteria. Moreso, nitrofurantoin can be used specifically to treat UTIs even in cases of vancomycin resistance. Vancomycin-resistant enterococci (VRE) are known to cause nosocomial infections.
Staphylococcus aureus
Staphylococcus aureus is an example of gram positive bacteria. It is catalase-positive, coagulase-positive cocci, and occurs in clusters. This bacterium is the most pathogenic staphylococci bacteria responsible for most staphylococci infections. S. aureus is known to cause pneumonia, inflammatory diseases, septic arthritis, skin infections, osteomyelitis, endocarditis, and abscesses. It can also cause scalded skin syndrome (exfoliative toxin), toxic shock syndrome (TSST-1), and food poisoning (enterotoxin).
Staphylococcus epidermidis
S. epidermidis is one of the gram-positive bacteria representative species. This bacterium is catalase-positive, coagulase-negative cocci in clusters. This species is novobiocin sensitive and commonly infects prosthetic devices and IV catheters, producing biofilms.
Staphylococcus saprophyticus
S. saprophyticus is a gram-positive, coagulase-negative, non-hemolytic coccus bacteria which is a normal flora of the genital tract and perineum. Staphylococcus saprophyticus being novobiocin resistant differentiates it from the other coagulase-negative staphylococci (S. epidermidis).
This bacterium is a common cause of uncomplicated urinary tract infections (UTIs), especially in young sexually active females. It accounts for the second most common cause of community-acquired UTI after Escherichia coli. Other complications such as acute pyelonephritis, epididymitis, prostatitis, and urethritis can be caused by Staphylococcus saprophyticus.
Streptococcus pneumoniae
Streptococcus pneumoniae is a gram-positive, encapsulated, lancet-shaped diplococci bacteria. This bacterium is the most common cause of community-acquired pneumonia, as well as otitis media, sinusitis, pink eye (conjunctivitis), and meningitis.
Streptococcus viridans
S. viridans inhabits the mucous membrane-lined cavities of humans and animals. Viridans streptococci consist of Strep. mutans and Strep. mitis and form part of the normal flora of the oropharynx and oral cavity. Also, it is found in the upper respiratory tract, all the regions of the gastrointestinal tract, and the female genital tract. These bacteria commonly cause dental caries and subacute bacterial endocarditis.
Streptococcus pyogenes
S. pyogenes is a gram-positive group A cocci. This is one of the examples of gram positive bacteria that can cause pyogenic infections such as erysipelas, pharyngitis, impetigo, and cellulitis. Also, they are known to cause toxigenic infections (scarlet fever, necrotizing fasciitis), and immunologic infections (glomerulonephritis and rheumatic fever). In order to detect S. pyogenes infections, Antistreptolysin O (ASO) titer can be used. ASO titer is a blood test that measures the antibodies produced against a substance called streptolysin O. This substance is produced by group A streptococcus bacteria.
Streptococcus agalactiae
Another common gram positive bacteria representative species is the Streptococcus agalactiae. This bacterium is a gram-positive group B cocci that colonize the vagina. Also, it is found mostly in babies and as a result, there is always a need for pregnant women to screen for Group-B Strep (GBS) at 35-37 weeks of gestation. These bacteria are known to cause sepsis, pneumonia, meningitis, and pyarthrosis.
Clostridia
Clostridia is one example of gram positive bacteria that are spore-forming rods. These gram positive rods include species such as C. tetani, C. botulinum, C. perfringens, and C. difficile. About 30 Clostridia species form toxins and cause disease in humans. These bacteria are usually involved with foodborne illnesses.
Clostridium botulinum forms spores that produce the botulinum toxin. This is the most dangerous toxin to humans as this toxin leads to various kinds of botulism, with foodborne botulism being the most common.
Clostridium perfringens, on the other hand, are usually associated with meat production and processing. Consuming meat contaminated by this bacterium can lead to food poisoning with symptoms like diarrhea and abdominal cramps within 6-24 hours of ingesting the contaminated food.
Clostridium difficile normally affects older individuals in the hospital. It usually occurs after taking antibiotics, causing conditions such as colitis, abdominal cramping, and severe diarrhea.
Clostridium tetani form spores that can be found in ash, soil, or on rusty tools. These spores produce tetanus toxin which is a neurotoxic substance that causes infection. It is called tetanus when the toxin causes an infection which calls for a serious medical emergency.
Bacillus anthracis
B. anthracis is one of the gram positive bacteria examples. This is one of the spore-forming gram positive rods. It produces anthrax toxin that causes serious illness in humans. Humans can get the toxin by contact with infected animals or through inhalation which results in an ulcer with a black eschar.
Some symptoms can occur based on how the anthrax is spread. Symptoms may include itchy bump that turns into a sore with a black center, nausea, coughing up blood, high fever, abdominal pain, and vomiting.
Bacillus cereus
B. cereusis a gram-positive rod found in soil and some foods. This spore-forming bacterium tends to cause illness when its spores survive under-cooked or reheated rice. Symptoms associated with B. cereusis include nausea, vomiting, and watery non-bloody diarrhea. Moreso, it causes wound infections, respiratory infections, and endophthalmitis.
Corynebacterium diphtheria
C. diphtheria is an example of gram-positive bacteria. This club-shaped rod is known to cause a variety of diseases. Corynebacterium diphtheriae is the main pathogenic bacterium among the estimated 30 Corynebacterium bacteria associated with human disease. This bacterium can cause respiratory infections, pseudomembranous pharyngitis, diphtheria, myocarditis, septic arthritis, arrhythmias, osteomyelitis, cutaneous infections, and endocarditis. However, Toxoid vaccines can be used to prevent diphtheria.
Listeria monocytogenes
L. monocytogenes is the only pathogenic Listeria bacteria. The infection of this gram-positive bacilli is as a result of ingesting cold deli meats and unpasteurized dairy products. Also, the bacterium can be acquired by a vaginal transmission during birth. Listeria monocytogenes cause mild symptoms of foodborne illness in healthy people whereas, in people with weakened immune systems, it can cause life-threatening conditions. It is known to cause neonatal meningitis, meningitis in immunocompromised patients, gastroenteritis, listeriosis, and septicemia. Nevertheless, it can be treated with ampicillin.
Infection
There are many pathogenic gram-positive bacteria that cause diseases in humans. Though there are more than 100 gram-positive bacteria that are pathogens, we will be looking at the few most notable species. The table below shows some examples of gram positive bacteria and the diseases they cause:
Gram positive bacteria and their diseases
Type of pathogenic gram positive bacteria | Examples of diseases caused by gram positive bacteria | |
1 | Staphylococcus aureus | Skin infections (cellulitis and folliculitis), septic arthritis, abscesses, endocarditis, bacterial pneumonia, food poisoning, toxic shock syndrome, scalded skin syndrome, staph infection |
2 | Staphylococcus epidermidis | Bacteremia, mediastinitis, surgical site infections, eye keratitis, endophthalmitis (inner eye infection) |
3 | Staphylococcus saprophyticus | Acute pyelonephritis, epididymitis, prostatitis, urethritis, uncomplicated urinary tract infections (most common), epididymitis |
4 | Streptococcus pneumoniae | Pneumonia, otitis media, sinusitis, pink eye (conjunctivitis), sinus infections, meningitis |
5 | Streptococcus pyogenes | Erysipelas, strep throat, cellulitis, pharyngitis, impetigo, scarlet fever, rheumatic fever, necrotizing fasciitis, glomerulonephritis |
6 | Streptococcus agalactiae | Sepsis, pneumonia, meningitis, pyarthrosis |
7 | Streptococcus viridans | Dental caries, subacute bacterial endocarditis, sepsis, pneumonia, meningitis |
8 | Enterococcus | Urinary tract infections, biliary tract infections, bacterial endocarditis, spontaneous bacterial peritonitis, diverticulitis, meningitis, bacteremia |
9 | Micrococcus | Cavitating pneumonia (immunosuppressed patients), septic arthritis, recurrent bacteremia, meningitis, septic shock, endocarditis. |
10 | Bacillus anthracis | Anthrax |
11 | Bacillus cereus | Wound infections, respiratory infections, endophthalmitis |
12 | Clostridium botulinum | Foodborne botulism (most common), wound botulism, infant botulism, inhalation botulism |
13 | Clostridium perfringens | Food poisoning, clostridial myonecrosis (gas gangrene) |
14 | Clostridium difficile | Colitis, abdominal cramping, severe diarrhea |
15 | Clostridium tetani | Tetanus |
16 | Listeria monocytogenes | Neonatal meningitis, meningitis in immunocompromised patients, gastroenteritis, listeriosis, septicemia |
17 | Corynebacterium diphtheriae | Diphtheria, pharyngitis, respiratory infections, septic arthritis, cutaneous infections, osteomyelitis, endocarditis |
Treatment
Gram positive bacteria treatment involves the use of antibiotics, fluid therapy, or antitoxins. Nevertheless, when treating gram-positive bacteria infection, a treatment option would depend on the following factors:
- Type of bacteria
- Antimicrobial resistance
- Whether the bacteria forms toxins
List of antibiotics that affect gram positive bacteria
- Penicillin
- Erythromycin
- Trimethoprim/sulfamethoxazole
- Clindamycin
- Doxycycline
- Vancomycin
- Linezolid
- Daptomycin
- Tigecycline
- Glycopeptides
- Amikacin
- Carbapenems
- Gentamycin
Antibiotics stop bacterial infections by interfering with the bacterial peptidoglycan layer which kills the bacterium or by inhibiting the bacterium from copying itself (reproducing). Here are some gram positive bacteria antibiotics and when they are used:
Penicillin
Penicillin is one of the major antibiotics that affect gram-positive bacteria. It was the first antibiotic ever introduced. Penicillin was introduced by Alexander Fleming in 1928 during World War II. This antibiotic is used mainly for streptococcal infections. Hence, it doesn’t cover Staph or Enterococcus infections. It is used to treat Streptococcus infections such as strep throat, sinus infections, urinary tract infections, and cellulitis.
The penicillinase-resistant organisms (cloxacillin, nafcillin, oxacillin, dicloxacillin) are used for Staph (MSSA) and Strep. Moreso, there are anti-pseudomonal penicillins that are effective against gram-positive, gram-negative, pseudomonas, and anaerobes. These anti-pseudomonal penicillins include piperacillin and ticarcillin.
Erythromycin
This is another strong antibiotic used to treat gram-positive bacterial infections. Erythromycin belongs to a class of antibiotics called macrolides, the same class as azithromycin and clarithromycin. It is usually prescribed for people that are allergic to penicillin. This antibiotic stops the growth of the bacterium and is effective for both gram positive bacteria and gram negative bacteria. Erythromycin is used to treat gram-positive infections like bacterial pneumonia, pink eye, strep throat, and staph skin infections.
Trimethoprim/sulfamethoxazole
One of the gram-positive bacteria antibiotics is Trimethoprim. These oral antibiotics are used to treat mild to moderate Methicillin-resistant Staphylococcus aureus (MRSA) infections. However, it has been noticed that trimethoprim/sulfamethoxazole increases warfarin levels which leads to an increased international normalized ratio (INR).
Clindamycin
Clindamycin is also an oral antibiotic used to treat mild-to-moderate MRSA infections.
Doxycycline
This oral antibiotic can be used for the treatment of mild to moderate Methicillin-resistant Staphylococcus aureus (MRSA) infections.
Vancomycin
Vancomycin is one of the gram-positive bacteria antibiotics used to treat moderate-to-severe community and hospital-acquired Methicillin-resistant Staphylococcus aureus infections. This antibiotic needs renal dosing with trough levels between 15-20.
Linezolid
This is one of the antibiotics that affect gram positive bacteria. It can also be used for the treatment of moderate to severe community and hospital-acquired MRSA. This antibiotic usually becomes an option if the patient is allergic to vancomycin. Also, it is one of the options used to treat vancomycin-resistant enterococci.
Daptomycin
This antibiotic is also used to treat infections caused by gram-positive bacteria. It is mostly used to treat vancomycin-resistant enterococci.
Tigecycline
This antibiotic is one of the options for the treatment of vancomycin-resistant enterococci.
Glycopeptides
One of the common antibiotics for gram positive bacteria that is used to treat serious infections caused by drug-resistant bacteria is Glycopeptides. This antibiotic destroys the bacterial cell wall as penicillin does. It can be used to treat gram positive bacteria infections like multidrug-resistant pneumonia, MRSA, and colitis.
Amikacin
Amikacin is a good antibiotic medication used for the treatment of several bacterial infections such as meningitis, joint infections, pneumonia, intra-abdominal infections, sepsis, and urinary tract infections. In fact, amikacin appears to be one of the most effective antibiotics for gram positive bacteria uti treatment.
Carbapenems
This is a class of highly effective antibiotic agents that are usually used to treat severe or high-risk bacterial infections. The antibiotic covers gram-positives, gram negatives, and anaerobes. It is usually used for suspected or known multidrug-resistant (MDR) bacterial infections.
Gentamicin
Gentamicin is another antibiotic used to treat severe or serious bacterial infections. It is another effective antibiotic for gram positive bacteria UTI treatment.
Fluid therapy
In some cases of bacterial infection, fluid therapy may be recommended as part of the gram positive bacteria treatment option. This helps to replenish the fluid levels of the body and prevent dehydration. Fluid management is generally needed to treat bacterial conditions caused by toxins.
Antitoxin
Treatment of toxin-related illnesses such as anthrax and botulism will require antitoxin. Antitoxins work by targeting and removing the toxins in the body. The appropriate antitoxin used is dependent on the specific toxin. Moreso, this medicine is used in combination with other treatments.
Identification
Based on their various characteristics, gram-positive organisms can be identified and classified. In biology, students and professionals use a dichotomous key to identify and classify these bacteria into specific categories. Using a dichotomous key is the most commonly used form of classification or identification key used in biology to identify unknown bacterial cells.
Here is a link to a printable form of dichotomous key for gram positive bacteria in PDF format that can be used for their identification and classification. Also as a tutor or educator, you can make a dichotomous key for gram positive bacteria, Watch the video below on how to make one.
Gram positive bacteria vs Gram negative bacteria
The major difference between gram negative and gram positive bacteria is the thickness of the peptidoglycan layer and the presence or absence of the outer lipid membrane. Gram-positive bacteria have thicker peptidoglycan cell wall structure and stain purple/blue in a gram stain test. Whereas, gram-negative bacteria have a thin peptidoglycan cell wall and stain red to pink in the gram stain test.
The cell walls of gram-positive bacteria contain peptidoglycan, lipid, teichuronic acid, and teichoic acid. This structural component is different from the gram-negative bacteria cell wall that is made up of peptidoglycan, and the outer membrane (that consists of lipid, protein, and lipopolysaccharides). Despite gram-positive bacteria having a thicker peptidoglycan layer, they are more susceptible to certain cell walls targeting antibiotics than gram-negative bacteria because they lack an outer membrane.
Gram-negative bacteria are therefore more resistant to antibiotics than gram-positive bacteria. They are more resistant to a wide range of antibiotics because of their outer membrane. Gram-positive cells are easier to kill because their thick peptidoglycan layer absorbs antibiotics and cleaning agents easily. Gram-negative cells, on the other hand, have a thin peptidoglycan layer and do not absorb any foreign material surrounding them.
The majority of antibiotics, in order to access their targets, must pass the outer membrane. For instance, hydrophilic antibiotics pass through porins. Therefore, gram-negative bacteria can alter their outer membrane by changing their hydrophobic properties or by mutations in porins. This creates resistance for these bacterial cells. Gram-positive bacteria lack this factor and thus are more susceptible to antibiotics.
FAQs
What does gram positive bacteria mean?
Bacteria species that stain purple/ blue after the gram staining test are said to be gram-positive bacteria. When treated with gram stain, gram-positive bacteria appear purple under the microscope.
Why do gram positive bacteria stain purple?
Gram-positive bacteria stain purple because they take up the crystal stain used in the Gram stain test. This is attributed to the structure of their cell wall. The cell walls of gram-positive bacteria contain thick peptidoglycan layers that retain the primary stain of the crystal violet used.
After staining with the crystal violet stain, a mordant is applied to fix the dye on the cell. Then, the cell is decolorized with alcohol. Even after the bacteria has been decolorized with alcohol, it still retains the primary stain and appears purple under the microscope.
Are gram positive bacteria more resistant to antibiotics?
No, they are not. Gram-negative bacteria are more resistant to a wide range of antibiotics compared to gram-positive bacteria. They are more resistant to antibiotics because of their outer membrane.
Gram-positive bacteria are easier to kill because their thick peptidoglycan layer absorbs antibiotics and cleaning agents easily. Gram-negative bacteria, on the other hand, have a thin peptidoglycan layer and do not absorb any foreign material surrounding it.
Do gram positive bacteria have peptidoglycan?
Yes. Gram positive bacteria have a thick layer of peptidoglycan. The cell walls of gram-positive bacteria contain a 20-80 nm thick layer of peptidoglycan. This peptidoglycan is the molecule responsible for the bacteria retaining the gram stain.
Do gram positive bacteria have a cell wall?
Yes, they do. The cell walls of gram-positive bacteria contain peptidoglycan, lipid, teichuronic acid, and teichoic acid whereas the gram-negative bacteria cell wall is made up of peptidoglycan, and the outer membrane (that consists of lipid, protein, and lipopolysaccharides).
Do gram positive bacteria have endotoxins?
No. Endotoxins are not associated with gram positive bacteria. These bacteria do not have endotoxins because they lack an outer membrane. Gram-negative bacteria, on the other hand, produce endotoxins.
These endotoxins are part of the outer membrane of gram-negative bacterial cells which are liberated only when the cell lyses or the bacteria dies. Endotoxins are heat stable lipopolysaccharide-protein complexes that form the cell wall structure of gram-negative bacteria.
What color do gram positive bacteria stain?
They stain purple/ blue after being treated with the gram stain.
Can gram positive bacteria ferment lactose?
Gram-positive bacteria in a different formulation where bile salt and crystal violet are not incorporated in a MacConkey agar can also appear as lactose fermenters, though they are smaller in size than the gram-negative bacteria.
Do gram positive bacteria have an outer membrane?
No, they don’t have an outer membrane. These bacteria lack an outer membrane but are surrounded by thicker layers of peptidoglycan than in the gram-negative cells.
Which color indicates gram positive bacteria?
Stained gram-positive bacteria appear purple/ blue under the microscope while the gram-negative bacteria take up the counterstain color and appear red or pink.
Do gram positive bacteria produce endotoxins?
No. The gram-positive bacteria do not produce endotoxins because they lack an outer membrane.
Where are gram positive bacteria found?
Depending on the gram-positive species, they can be found in the soil, aquatic sediments, dust, skin, mouth, intestinal tract, or genital tract of humans.
Why are gram positive bacteria more susceptible to antibiotics?
Despite gram-positive bacteria having a thicker peptidoglycan layer, they are more susceptible to certain cell walls targeting antibiotics than gram-negative bacteria because they lack an outer membrane.
The majority of antibiotics, in order to access their targets, must pass the outer membrane. For instance, hydrophilic antibiotics pass through porins. Therefore, gram-negative bacteria can alter their outer membrane by changing their hydrophobic properties or by mutations in porins. This creates resistance for these bacterial cells. Gram-positive bacteria lack this factor and thus gram-negative bacteria are more resistant to antibiotics than them.
Do gram positive bacteria have porins
Yes. Initially, porins were first discovered in gram-negative bacteria, but currently, both types of porins have been found in gram-positive bacteria. Since these bacteria lack outer membranes, the porin channels are bound instead to specific lipids within the cell walls.
Do gram positive bacteria have lipopolysaccharides (lps)?
Gram-positive bacteria do not have lipopolysaccharides in their cell walls. Rather, their cell wall is composed of teichoic acids, lipoteichoic acids, and peptidoglycan.
What is gram positive bacteria in urine?
The presence of gram-positive bacteria in urine indicates a urinary tract infection. Amikacin and gentamicin appear to be some of the most effective antibiotics for gram-positive bacteria UTI treatment.
What differentiates gram positive bacteria from gram negative bacteria?
The main features that differentiate the gram-positive bacteria from gram-negative bacteria are the thickness of the peptidoglycan layer and the presence or absence of the outer lipid membrane.
Do gram positive bacteria have pili?
Some gram-positive bacterial cells have pili. The short and thin pili have been found on Streptococcus species, whereas the longer and flexible pili have been found on Corynebacterium species and pathogenic streptococci.
Are gram positive bacteria pathogenic?
Yes, the majority of gram-positive bacteria are pathogenic. Examples of pathogenic gram-positive bacteria include Micrococcus, Enterococci, Staphylococcus aureus, Staphylococcus epidermidis, Staphylococcus saprophyticus, Streptococcus pneumoniae, Streptococcus viridans, Streptococcus pyogenes, Streptococcus agalactiae, Clostridium tetani, Clostridium botulinum, Clostridium perfringens, Clostridium difficile, Bacillus anthracis, Corynebacterium diphtheria, Listeria monocytogenes, etc.