The Direct Coombs Test (DCT Test) is also called Direct Antiglobulin Test (DAT Test). The direct Coombs test was the older term used to describe this test and it is a test used to detect antibodies or complement against red blood cells (RBCs). The presence of these antibodies or complement on the red blood cells cause the destruction of the RBCs. The DAT Test or DCT test is positive in Hemolytic disease of the newborn, autoimmune hemolytic anemia or drug-induced immune hemolytic anemia and hemolytic transfusion reactions.
Table of Contents
- Significance of Direct Coombs Test
- Why is Direct Coombs Test done? Indications for requesting for a direct Coombs test to be done
- Direct Coombs Test Procedure
- Increasing the sensitivity of direct Coombs test
- Interpretation and Analysis of Direct Coombs Test
- Reasons why there may be false-negative direct Coombs test
- False Positive direct coombs test
- DAT Test Sensitivity
- What causes a Positive Direct Coombs Test (DAT Positive)
Significance of Direct Coombs Test
The direct antiglobulin test is use to identify whether there are antibodies in the blood that may destroy the RBCs. In order to understand the significance of the DCT Test (or DAT test), you need to understand what is normal and that which is abnormal this is explained below:
In your blood, there is a fluid called Serum and in this serum are suspended blood cells such as the Red blood cells (RBCs) and White blood cells (WBCs) and Platelets. What we are more interested in while explaining DAT test is the RBCs. The Antibodies are proteins in the body that help fight infections or any foreign organisms in the body and these Antibodies can help get rid of other cells that are not of your body such as fighting bacteria cells, Viruses, Fungi, and many more. This work of antibodies is good because what is not of the body is removed. In the DAT test, what these antibodies do is that the bind to any Red blood cell that the body sees as not of the body and destroy them. The reaction of these antibodies to these RBCs is what is seen physically as Positive DCT test or Positive DAT test which signifies the presence of antibodies against Red blood cells in the blood.
Why is Direct Coombs Test done? Indications for requesting for a direct Coombs test to be done
- Direct Coombs test is useful in Antibody identification: the DCT test can be used to evaluate unexpected antibodies.
- It is used in the diagnosis of Autoimmune hemolytic anemia: this shows the presence of IgG and/or complement coating the RBCs. A positive direct antiglobulin test with IgG (with or without complement) and a panagglutinin eluate is consistent with the diagnosis of warm autoimmune hemolytic anemia whereas a direct antiglobulin test positive with complement only, is seen in patients with cold agglutinin disease.
- Direct Antiglobulin test helps in the diagnosis of Drug-induced hemolytic Anemia
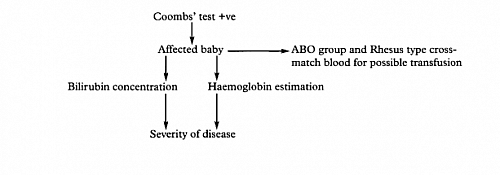
- Useful in the diagnosis of Hemolytic disease of the fetus and newborn (HDFN): this is performed to evaluate the presence of HDFN. A neonatal blood sample should have a direct coombs test performed if the mother has a positive antibody screen. The direct coombs test may also be indicated when the mother is ABO-incompatible with the neonate such as the blood group of the mother being group O and the newborn being group A.
- Useful in the evaluation of Transfusion reactions: a DCT test is performed on any post-transfusion sample that there was transfusion reaction in order to evaluate the possible cause of the acute or delayed hemolytic transfusion reaction which may be due to uncross matched blood or poorly cross matched blood samples.
Direct Coombs Test Procedure
- Specimens must be blood samples anticoagulated with EDTA to prevent clotting
- Direct Coombs Test can initially be performed with a polyspecific anti-human globulin reagent, which contains anti-IgG and anti-C3d and may also contain antibodies to other C3 determinants (C3dg, C3b, C3c) and other immunoglobulins (Iga, IgM).
- If there is positive direct coombs test when the polyspecific reagent is used, then the sample can be retested with monospecific anti-IgG and anti-C3d/C3dg reagents to further characterize the reactivity. These reagents are licensed in the Unites States by the FDA.
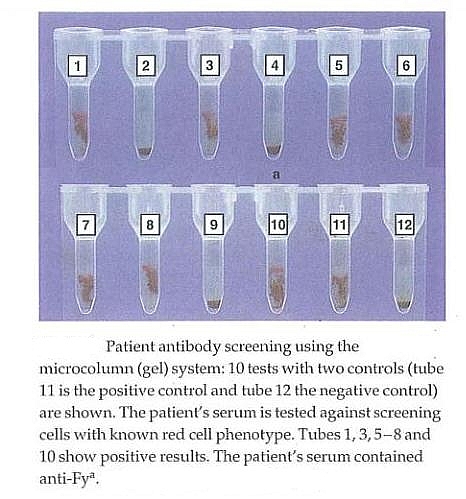
- Direct Antiglobulin Test can be performed with a variety of serologic techniques, such as tube (wet), microtube columns (gel) and solid phase methods.
- Cells from cord blood are suspended with the reagent and if the baby is affected (has maternal antibody attached) agglutination will occur. This test detects the antibodies absorbed to the RBCs. A positive direct antiglobulin (DAT or Coombs) test identifies in vivo antibody-coated and complement-coated red cells. A positive DAT distinguishes AIHA from other types of hemolytic anemia that produce spherocytes.
The sensitivity and specificity of the direct antiglobulin test performed by the gel test is 74 to 98% while that of the tube test is about 89 to 95%.
Increasing the sensitivity of direct Coombs test
Increasing the sensitivity of direct Coombs test can be done using a chemical called an Eluate. This helps in antibody identification by concentrating the amount of antibodies. There are commercial elution kits available. The process of removing these antibodies from the RBCs in order to increase concentration and hence increase sensitivity can be done using different techniques such as freezing and thawing, heating, use of cold acid, dicholormethane glycine-HCl/EDTA and digitonin acid. Reactivity of eluates can be enhanced by use of polyethylene glycol (PEG).
Interpretation and Analysis of Direct Coombs Test
The interpretation of the direct antiglobulin test when positive depends on the clinical context of the patient, such as the underlying diagnosis, drug history, pregnancy, history of previous blood transfusion history and presence of unexplained hemolytic anemia. The significance of positive direct Coombs test needs to be assessed together with the clinical and laboratory information whether there is presence of hemolysis or not. Further evaluation may be necessary in patients who have evidence of hemolytic anemia, patients receiving medications associated with a positive DCT test (such as Cephalosporins and Penicillin), patients with transfusion within the last 3 months and those who received a solid organ transplantation.
Reasons why there may be false-negative direct Coombs test
- When the antibody causing the immune hemolysis is not IgG or IgM, because the polyspecific reagent used in testing may not have the appropriate specificity for the immunoglobulin causing the hemolysis.
- There could be false negative Coombs test when the amount of IgG bound to RBCs is too low. The concentration may be too low for the reagent to detect its presence. When this occurs, more sensitive techniques can be used.
- Incorrect washing or resuspending, or delayed testing, may result in a false-negative Direct antiglobulin test.
False Positive direct coombs test
False-positive Coombs test may occur when red blood cells used are from clotted specimens (especially when the specimens have been refrigerated) – this is due to false complement reactivity.
DAT Test Sensitivity
The DAT test can detect a minimal level of 100500 IgG molecules/RBC and 4001100 C3d molecules/RBC, depending on the method and testing techniques. The direct coombs test detects the presence of IgG and/or C3 (when IgG binds to RBCs it fixes complement, which is more readily detected than IgM) coating red blood cells (RBCs) in vivo.
Why is the direct Coombs test frequently negative or weakly positive in Newborns/infants with ABO incompatibility?
The direct Coombs test is frequently negative or weakly positive in Newborns with ABO incompatibility because there are fewer A or B antigenic sites on the newborn red blood cell (RBC) with a greater distance between antigenic sites compared with adult RBCs. In addition, there is absorption of serum antibody by ABO antigens located on tissues throughout the body.
What is the most important test to establish the diagnosis of Auto-Immune Hemolytic Anemia (AIHA)?
The Coombs test or direct antiglobulin test (DAT). The diagnosis of AIHA requires the presence of autoantibodies that bind to Red blood cells and signs or symptoms of hemolysis. However, about 10% of patients with AIHA show Coombs negative result, therefore, patients should be treated for AIHA if the disease is strongly suspected, even if the direct Coombs test is negative.
What causes a Positive Direct Coombs Test (DAT Positive)
- Autoantibodies directed at Red cells antigens such as in warm autoimmune hemolytic anemia and cold agglutinin syndrome
- Alloantibodies in a patient who was recently transfused antigen-positive RBCs (acute or delayed hemolytic transfusion reaction)
- Passively transfused alloantibodies against the patients RBCs resulting from plasma-containing components (platelet component) or a plasma derivative (intravenous immunoglobulin or Rhesus immune globulin)
- Alloantibodies in the maternal circulation which cross the placenta and coat the fetal Red cells such as in hemolytic disease of the fetus and newborn
- Antibodies against drugs which bind to the Red blood cells like Penicillin
- Absorbed proteins (IgG) which attach to altered Red blood cells membrane or RBCs modified by drugs like Cephalosporins
- Immune complex or complement binding to RBCs after drug administration secondary to a drug/anti-drug interaction like Quinidine or Phenacetin
- Nonspecific uptake of protein, usually IgG such as in patients with hypergammaglobulinemia or recipients of high dose intravenous immunoglobulin
- Antibodies derived from passenger lymphocytes as a result of either solid organ or hematopoietic progenitor cells transplantation
What does Direct Coombs positive mean?
A positive direct Coombs test does not necessarily imply that hemolysis is actively occurring. All it entails is that there are antibodies against the red blood cells.
What does a negative Direct Coombs Test mean?
A negative direct antiglobulin test does not exclude hemolysis. It could arise as a result of false negative test which could be due to clotted samples being used.