Table of Contents
What is Amenorrhea?
Amenorrhea or Amenorrhoea can be defined as the absence of period in women; this is mostly caused by Pregnancy but there are other causes other than Pregnancy. When there is no period and you are not pregnant, it means you have Amenorrhea but the cause must be known.
It is the absence of menstruation, which might be a temporary or permanent cessation of menses and may occur as a normal physiological condition such as before puberty, during pregnancy, lactation or menopause, or as a feature of a systemic or gynecological disorder.
Amenorrhea Types
- Physiological amenorrhea
- Pathological amenorrhea
It can be classified under two categories: Physiological (which includes Pre-puberty, Pregnancy, and Post-menopausal or Menopause related) and Pathological (which is further divided into Primary and Secondary Amenorrhea).
Physiological Amenorrhea (Normal Amenorrhea)
- Pre-puberty: this type occurs during Puberty (ages 10 to 16 years); it is normal and said to be physiological; however, if there is no period even after the age of 16 years, then the cause should be investigated.
- Pregnancy: it is expected that no bleeding should occur during pregnancy.
- Postpartum period (Lactational Amenorrhea): Breastfeeding following childbirth has been known to be a form of contraception and Amenorrhea is expected for a variable phase following delivery, particularly in association with mothers who are breastfeeding because prolactin is secreted in large quantities by the anterior pituitary in breastfeeding mothers and this causes partial suppression of luteinizing hormone (LH) production so that ovarian follicles may grow, this also prevents ovulation, and therefore results in Amenorrhea. If the mother does not breastfeed the baby then menstruation usually returns after 2 to 3 months and only prolongs when she breastfeeds regularly.
- Menopause: This is the last menstrual period and can only be recognized in retrospect; it is being diagnosed after amenorrhea for a year. Menopause signifies the end of the reproductive life of a woman and any bleeding occurring after this is abnormal unless the woman is taking cyclical hormone replacement therapy (HRT).
Pathological Amenorrhea
- Primary Amenorrhea
- Secondary Amenorrhea
Primary
Primary amenorrhea is defined as the failure to commence a menstrual period after the age of 16 years; this requires systematic investigation if the correct diagnosis is to be made.
Secondary
This is the absence of menses for a period of 6 months in a woman who has once had menstrual periods before. Secondary amenorrhea is used to describe menstrual absence in those who had been menstruating earlier but not have stopped for a period of 6 months because of a disease process or a disorder affecting the menstrual flow.
Treatment
Treatment of Amenorrhea depends on the type and the cause. Each type will be discussed with the possible treatment below. Some causes are due to congenital abnormalities and may just be managed but cannot be cured.
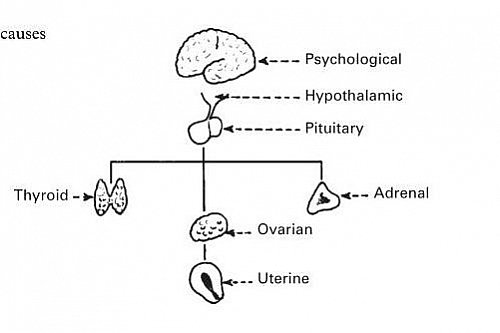
What Causes Amenorrhea?
- Uterine or lower genital tract causes
- Ovarian causes
- Pituitary causes
- Hypothalamic causes
Causes from the uterine or lower genital tract
- Imperforate hymen or Transverse vaginal septum: this causes primary amenorrhea in which there is no visible bleeding, although the usual menstrual cycle symptoms are present
- Ashermans Syndrome: In Ashermans syndrome, the uterine cavity is obliterated by adhesions that may be due to surgery such as dilatation and curettage for termination of pregnancy or it may be due to infections such as tuberculosis or Schistosomiasis in developing countries.
- Congenital Androgen Insensitivity: this was initially called Testicular feminisation syndrome Congenital androgen insensitivity is the third commonest cause of primary amenorrhea; the individual appears physically as a female but the uterus is absent. The karyotype is 46XY.
- Mullerian Agenesis: by the 10th week of gestation, the Mullerian ducts fuse to form the fallopian tubes, uterus, and upper portion of the vaginal tissue. A lack of development of this duct will lead to the absence of the structures mentioned.
Signs and Symptoms caused by imperforate hymen
- Pelvic pain of increasing severity
- Urinary retention
- A pelvic mass is felt that may be visible
- The vaginal membrane or hymen is bulging
Treatment
Treatment of Amenorrhea caused by obstruction to flow is incision and drainage and if the septum is particularly thick, vaginal reconstruction may be required. For Ashermans syndrome, the adhesions should be broken down by hysteroscopy.
Ovarian causes of Amenorrhea
- Gonadal dysgenesis: Women with gonadal dysgenesis have abnormal ovarian development and therefore absence of ovaries or streak ovaries
- Premature ovarian failure: this occurs following depletion of ovarian follicles from the ovary before the normal age of menopause thereby leading to premature menopause with associated menopausal symptoms such as amenorrhea, hot flushes, loss of libido, etc. Women with premature ovarian failure should be advised that they are likely to be infertile, although spontaneous pregnancies have been reported. Pregnancy can be achieved by IVF (in vitro fertilization) with donor oocytes.
- Resistant ovary syndrome: in this condition, the ovarian follicles fail to develop, even though the circulating levels of gonadotropins are high. Treatment of this type of amenorrhea is the same as for premature ovarian failure
- Disorders of ovulation such as Polycystic Ovarian Syndrome (PCOS): this is a functional disorder of the hypothalamopituitary ovarian axis associated with anovulation. The symptoms and signs are highly variable such that Amenorrhea could occur in some while menorrhagia occurs in others. Other symptoms include oligomenorrhea, hirsutism, obesity, hirsutism, acne, and infertility.
- Hormone-producing tumors, such as granulosa cell tumors (estrogen-producing) or Leydig cell tumors (androgen-producing).
Pituitary causes
- Hyperprolactinemia: during pregnancy, there is a 10-fold increase in serum prolactin levels but non-physiological hyperprolactinemia occurring when a woman is not pregnant, can cause amenorrhea or galactorrhea (excessive production of breast milk) or both. Hyperprolactinemia is the main cause of amenorrhea in about 20% of women with this condition.
- Pituitary adenoma
- Craniopharyngioma
- Other tumors such as meningioma
- Pituitary necrosis (Sheehan’s syndrome/Simmonds disease).
Hypothalamic causes
Disorders of the hypothalamus result in hypogonoadotrophic hypogonadism, and hence amenorrhea. The patients have low gonadotropins, normal prolactin levels, a normal pituitary gland on radiological evaluation and they fail to bleed in response to progesterone.
Causes due to Hypothalamic disorders
- Anorexia nervosa: an eating disorder leading to very low body weight and amenorrhea
- Exercise: Female athletes are commonly amenorrhoeic due to suppression of GnRH production
- Kallmann’s syndrome: This is a rare condition of congenital hypogonadotrophic hypogonadism in association with anosmia (inability to perceive smell). Secondary sexual characteristics are absent but ovulation can be induced with gonadotrophins.
Diagnosis
Diagnosis of Amenorrhea is straightforward when there is an absence of menstrual period after the expected age (16 years for Primary amenorrhea) but more than 6 months for secondary amenorrhea. However, diagnosis of the specific cause of the type of Amenorrhea is what requires laboratory investigations to be done. The investigations and the expected results for diagnosis are outlined below.
Laboratory investigations
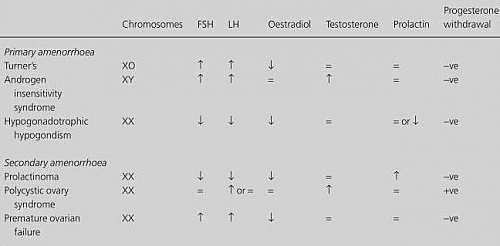
- Premature Ovarian Failure (POF) is diagnosed when there is elevated serum FSH levels (>20 IU/L) with elevated LH but low estradiol
- FSH, LH, and estradiol are all low in Hypothalamic hypogonadism
- Low levels of LH, FSH, and estradiol in Sheehan’s syndrome
- TSH is raised but T4 may be low or normal in Hypothyroidism
- Gonadal dysgenesis shows high levels of FSH and LH but low estradiol
- The polycystic ovarian syndrome shows high levels of LH with normal FSH and high or normal androgens
- Genital tract abnormalities can be seen on ultrasound scan
- CT scan of the pituitary gland will show any tumor
- Progestogen challenge test or Progesterone challenge test can be used to test for the presence of the uterus and the patency of the outflow tract. This test is done by administering a progestogen for 5 days and within 3 days of stopping there should be a withdrawal bleed. This implies that the endometrium has been primed with estrogen and that the uterus is present and that there is no outflow tract obstruction.
Medications for treatment
- Bromocriptine, Quinagolide, and Cabergoline are used in the treatment of amenorrhea caused by Hyperprolactinemia
- In PCOS (polycystic ovarian syndrome) fertility can usually be induced with clomifene and the use of combined oral contraceptive therapy will result in regular artificial bleeding.
Side effects
The complications or side effects of Amenorrhea depend on the cause of the amenorrhea include the following:
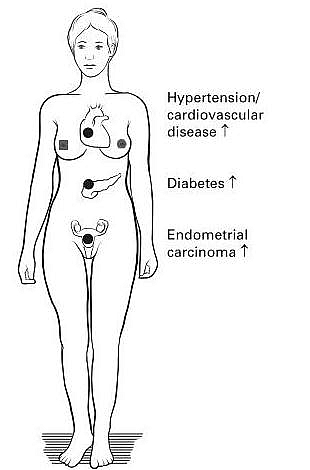
- Women with PCOS who are anovulatory are at increased risk of endometrial hyperplasia and subsequent endometrial cancer due to the high estrogen and low progesterone levels.
- The hyperinsulinemia associated with insulin resistance leads to an increased risk of diabetes mellitus in PCOS
- Women with PCOS who are obese and insulin-resistant have an increased risk of hypertension and cardiovascular disease
- Infertility
- Painful breasts for those with prolactinomas