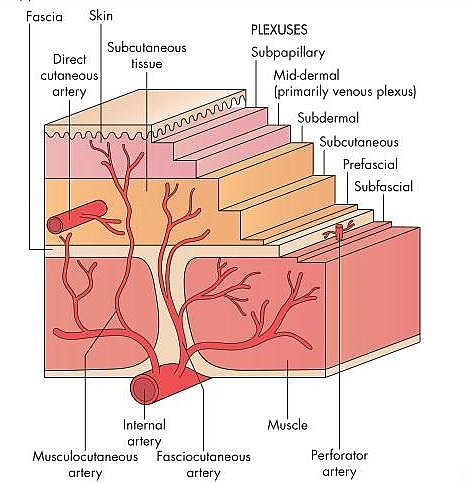
Skin Grafts are used to mainly to help in wound healing and also done when a part of the skin has been excised due to cancer. Skin grafting is a procedure whereby a part of the skin is harvested from and transferred to another part in order to help wound healing.
Table of Contents
- What is Skin Graft?
- Uses of Skin grafts
- Difference between skin graft and skin flap
- Differences between Skin graft and skin transplant
- Classification of skin grafts based on source of graft
- Classification of skin grafts based on timing
- Classification of skin grafts based on thickness of the skin tissue harvested
- Full Thickness Skin Graft (Wolfe Skin graft)
- Split Thickness Skin Grafts (also called Partial Thickness Skin Graft or Thiersch skin graft)
- Instruments used in Split thickness Skin grafts Procedure
- Advantages of Split Thickness Skin Grafts
- Disadvantages of Split Thickness Skin Grafts
- Split Thickness Skin Graft Technique (Steps in Partial thickness skin graft procedure)
- Classification of skin grafts based on mode of application of the graft
- What are the reasons for skin grafts? (Indications for skin grafts)
- Factors affecting Graft take
- The 3 phases of graft survival
- Skin Graft Recovery Time and Stages of Healing
What is Skin Graft?
A skin graft is the transfer of skin tissue from a donor site to a recipient site without its blood supply. The blood supply of the skin tissue from its site of origin is not harvested in a skin graft. Several tissues can be transferred and not only the skin. Other tissues that can be grafted include: bone grafts, cartilage grafts, tendon grafts, nerve grafts, muscle grafts, fat grafts and many others.
When more than one tissue is used in the process of grafting, it is referred to as Composite graft. An example is the grafting of skin and cartilage to another skin and cartilage at the same time.
Uses of Skin grafts
- To aid in wound healing
- To restore normal function of the skin tissue
- To restore normal anatomy (make the part of the body look normal even when the function is not restored. This is for cosmetic reasons) this could occur following burns
- To prevent skin contractures
- To release a contracture or relieve pain due to contracture or compression
When a skin deformity needs reconstruction, a skin graft or flap is employed to restore normal anatomy or function and also to employed when wounds cannot be closed by primary intention (when the edges of the wound are too wide and cannot be joined directly together except with additional skin from another part of the body).
Difference between skin graft and skin flap
In a skin graft, the blood supply of the harvested skin tissue is not taken whereas in a skin flap, the blood supply is harvested together with the skin tissue – this is the difference between a skin flap and a skin graft.
Differences between Skin graft and skin transplant
Skin graft should not be confused with skin transplant; Skin graft is a general term whenever a part of the skin is taken (from whatever location of the skin of the same person or from another person or even from an animal) whereas skin transplant is used to describe the transfer of skin tissue from one person to another or from an animal. This means you cannot use skin transplant when the skin tissue is harvested from the same person in a different part of the body in this case, it is called an autograft. You will understand the differences between skin graft and skin transplant when you see the types of skin grafts listed below.
Classification of skin grafts based on source of graft
- Autograft
- Isografts
- Allografts
- Xenografts
Autograft
When a skin tissue is harvested from one part of the body to another part of the body of the same individual
Isograft
When skin is taken from one individual to another who share the same genes such as identical twins or from cloned species with same genes
Allograft
When a graft is taken from one individual to another individual who are not genetically identical such as taking skin tissue from a mother to her child
Xenograft
When skin is taken from one species to another species such as use of porcine skin (skin of pig) used in burn wounds for humans
Classification of skin grafts based on timing
- Primary graft
- Delayed primary graft
- Secondary graft
Classification of skin grafts based on thickness of the skin tissue harvested
- Full Thickness skin graft or (Wolfe skin graft)
- Partial or Split Thickness skin graft- this is further classified into Thin partial thickness skin graft (also known as Thiersch skin graft), Intermediate partial thickness skin graft and Thick partial thickness skin graft.
Full Thickness Skin Graft (Wolfe Skin graft)
Full thickness skin graft involves harvesting the epidermis and the dermis of the skin in its entirety. The advantage that the full thickness skin graft offers is that it helps to maintain greater semblance to normal skin and has less risk of contracting.
Full thickness skin graft should be carried out in such a way that donor site scar should be along relaxed skin tension line. Recipient site thickness is an important consideration for donor area.
Best parts of the body to harvest for full thickness skin grafts
- For Nose grafts, best parts to harvest is the forehead or the pre-auricular area
- For Cheek grafts, best parts include the neck and supraclavicular area
- For Hand grafts, the best part to harvest is the groin area
The harvested skin is aggressively defatted to improve short term survival by imbibition; recipient site is dressed with bolster dressings like in split thickness graft.
Split Thickness Skin Grafts (also called Partial Thickness Skin Graft or Thiersch skin graft)
Split thickness skin grafts involve the harvesting of the epidermis and partial (or variable thickness) of the dermis. Thicker split thickness skin grafts require more optimal donor site condition to survive.
Best sites for taking graft tissue in split thickness skin grafts
- Commonest part used in split thickness skin grafts is the thigh
- Other parts include Leg, arm, forearm and scalp etc.
Instruments used in Split thickness Skin grafts Procedure
- Free hand grafting knife such as the Humby knife and Da-Silva knife: these knives are operator dependent and good when the wound area has an irregular edge and thickness
- Drum dermatome: used to harvest from irregular surface and shape
- Power dermatome used to harvest from parts with regular thickness
Advantages of Split Thickness Skin Grafts
- Used when a large area needed to be harvested
- When previous donor can be used
- It has a better take- the thinner the skin graft, the better the take
- The graft can be expanded by meshing
- It has less requirement for take
Disadvantages of Split Thickness Skin Grafts
- Not durable
- Secondary contracture can be severe – use of partial thickness skin graft in flexure area (areas of joints for movements forwards and backwards) has to be accompanied by prolonged splinting
- Hyperpigmentation both at donor and recipient site occurs
- Absent skin appendages such as sweat glands and sebaceous glands which may lead to dry skin
- It has poor cosmetic outcome
Split Thickness Skin Graft Technique (Steps in Partial thickness skin graft procedure)
- Routine cleaning
- Use lubricant (such as Vaseline from Vaseline gauze) – applied over donor area and cutting end of dermatome
- Set dermatome for thickness of graft
- Stretch skin with graft wood on both direction and take graft
- Apply pressure with gauze or cover donor area with adrenaline (1 in 200000)soaked gauze for hemostasis
- Apply bolster dressing consisting of non-adherent layer (sofra-tulle or vaseline gauze) then capillary layer (gauze), then absorbent layer (cotton wool). Which is then immobilized by applying crepe bandage, tie over sutures or use of Plaster of Paris (POP)
- The dressings should be left undisturbed for 5 days unless there is sign of infection (signs such as bad odor, pain, soaked dressings and fever).
- The Donor can have occlusive, semi-occlusive or semi-open dressings
Classification of skin grafts based on mode of application of the graft
- Sheets skin graft
- Meshed skin graft
- Postage stamps skin graft
What are the reasons for skin grafts? (Indications for skin grafts)
- When wound cannot be closed primarily
- Lack of adequate adjacent tissue to close a wound judged based on the quantity, quality, location and appearance of the adjacent tissue
- Uncertainty of tumor clearance
- Nutritional status of the individual graft will not take in malnourished individuals
- Age of the individual not good for elderly
- Smoking habits grafts may not take in a smoker
Factors affecting Graft take
- Viability of the recipient site: there should be adequate blood supply at the site that a grafted skin tissue is to be transferred to.
- Hemostasis: bleeding should be controlled as hematoma (a collection of blood causing swelling) causes graft failure
- Bacterial load: Excessive contamination (especially by beta hemolytic streptococcus) of a grafted skin leads to graft failure. Any infection of the recipient site by beta hemolytic Strep is an absolute contraindication for skin grafting
- Comorbidities: systemic diseases such as diabetes mellitus, use of some medications such as anticoagulants (blood thinning drugs)
- Local effects such as irradiation
- Local movements affects graft take
- Skin graft over tumor bed is not viable
A graft take refers to successful graft of which the purpose has been achieved and there is no failure of graft.
The 3 phases of graft survival
- Imbibition
- Inosculation
- Angiogenesis
Skin Graft Recovery Time and Stages of Healing
- Stage of Imbibition– Plasmatic imbibition is responsible for survival for 2-3 days until angiogenesis occurs
- Stage of Inosculation: this occurs in day 3; cut ends of the vessels under the dermis begin to form connection with those of the beds.
- Stage of Angiogenesis: by day 5 new blood vessels grow into graft and graft become vascularized