Wound Healing is the replacement of damaged or dead tissue by a living fibrous tissue. Wound healing is different from Regeneration which is the replacement of damaged tissue with another tissue that is similar like the damaged one and the replacement is indistinguishable. Regeneration occurs in lower animals such as earthworms but it does not occur in higher animals like humans.
Resolution can be distinguished from Wound healing in the sense that, resolution occurs when there is minimal damage to tissue with recovery and the end result being similar like the original tissue without formation of a new tissue this occurs in a blind boil under skin that resolves without the skin being damaged.
Table of Contents
How long does it take for a wound to heal?
There are different factors that influence the time it takes for wound to heal, and the time varies according to the type of tissue, its blood supply and viability with other associated comorbidities of the individual such as state of health or associated diseases and also the degree of the damage to the tissue.
Types of Wound Healing
- Healing by Primary intention or Primary Wound healing : this is the mechanical apposition of the wound edges; Normal healing with minimal scar.
- Healing by Secondary intention or Secondary wound healing: in this type, the wound heals by the process of inflammation, contraction and re-epithelialization by being left opened. There is increased inflammation and proliferation leading to poor scar formation
- Healing by Tertiary intention or Delayed Primary wound healing: in this type, the wound is left for a couple days to clean up and then close primarily by mechanical apposition of the edges
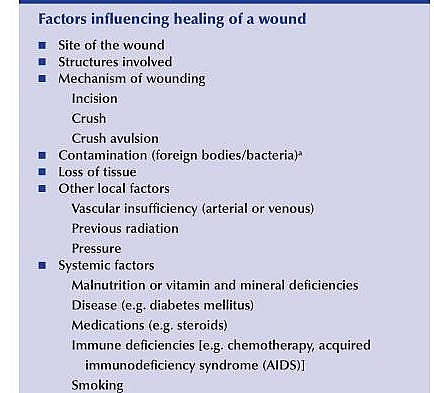
Factors influencing healing of a wound
- Site of the wound: wounds occurring at sites having good blood supply such as the scalp tend to heal faster than those without blood supply such as the bones.
- Structures involved: skin or tongue or intestines heal faster than when bones or cartilage is involved.
- Mechanism of wounding: Incision heals faster than crush or avulsion
- Presence of contamination by foreign bodies or bacteria delays wound healing
- Loss of tissue: when a tissue is lose, it takes longer for the wound to heal
- Smoking delays wound healing
Factors that delay wound healing
- Infection
- Poor vascularity
- Malnutrition such as Protein Energy Malnutrition (Kwashiorkor and Marasmus)
- Radiation
- Smoking
- Significant loss of tissue
- Use of cytotoxic drugs as they attack growing cells
- Diabetes mellitus
3 or 4 Phases of Wound Healing
- Inflammatory phase
- Proliferative phase
- Remodeling phase or the maturing phase
Some agree that there are 3 phases of wound healing while others agree to 4 phases of wound healing. For those with 4 phases, there is a hemostatic phase, which is referred to as occurring before the inflammatory phase or a destructive phase following inflammation consisting of the cellular cleansing of the wound by macrophages.
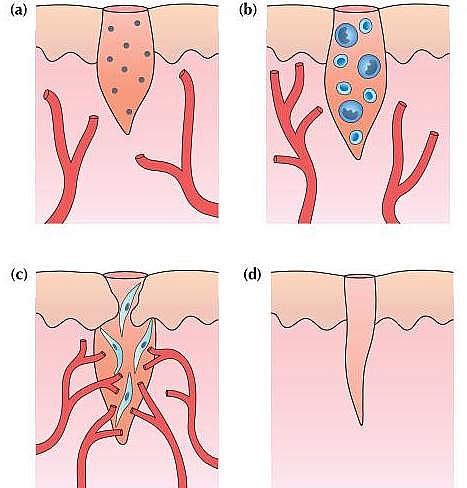
The inflammatory phase of wound healing
This stage begins immediately after wound occurs and may last for 2 to 3 days. It starts with bleeding, then vasoconstriction and formation of thrombus in order to limit blood loss. The thrombocytes (Platelets) stick to the damaged endothelial lining of vessels and relaease chemicals such as adenosine diphosphate (ADP) this causes thrombocytic aggregates to fill the wound. Further cytokines (chemicals that attract lymphocytes and macrophages) are released that attract inflammatory cells such as polymorphonuclear lymphocytes (PMN) and macrophages.
The macrophages then remove devitalized tissue and micro-organisms while regulating fibroblast activity in the proliferative phase of wound healing.
The Inflammatory phase of wound healing is the one commonly called Inflammation which is described using the following words: rubor (redness), tumor (swelling), calor (heat) and dolor (pain).
The proliferative phase of wound healing
This stage of wound healing lasts from the 3rd day to the 3rd week and consists of mainly fibroblast activity with the production of collagen and ground substance (glycosaminoglycans and proteoglycans), the growth of new blood vessels as capillary loops (angioneogenesis) and the re-epithelialization of the wound surface. Fibroblasts require vitamin C to produce collagen and it is the reason why there is delayed wound healing in malnutrition or when there is deficiency of Vitamin C; it is also because of this reason that patients are given vitamin C to aid in wound healing. Smoking inhibits wound healing by limiting the formation of collagen.
The wound tissue formed in the early part of proliferative phase is called granulation tissue. In the latter part of this phase, there is an increase in the tensile strength of the wound due to increased collagen, which is at first deposited in a random fashion and consists of type III collagen.
The remodeling phase of wound healing
This phase of wound healing is characterized by maturation of collagen (type I replacing type III until a ratio of 4:1 is achieved). There is also a realignment of collagen fibers along the lines of tension, decreased wound vascularity and wound contraction due to fibroblast and myofibroblast activity. It is the excessiveness of this phase of wound healing that leads to formation of Keloids and hypertrophic scars.
Complications of Wound healing
- Hypertrophic Scars and Keloid
- Formation of adhesions
- Contractures
- Cirrhosis such as in liver cirrhosis this occurs because the liver tries to regenerate