The GCS was originally devised in 1974 to assess the level of consciousness after head injury, though now is used for almost all acutely presenting patients. It is widely used and accepted in Medicine as a very useful tool in determining the level of consciousness of patients with both traumatic and non-traumatic forms of coma. The GCS should not be confused with the Glascow Outcome Scale (GOS). The GOS determine the level of disability or outcome at the time of hospital discharge.
The GCS is helpful in following the progress of patients. It was initially used for adults only but can be applied to children between 4 to 15 years of age. Children less than 4 years can be assessed by other coma scales such as the Blantyre coma scale and the AVPU score. This is important because the GCS relies on the level of comprehension of speech of which children of less than 4 years may not comprehend speech very well.
The Glascow coma scale provides for evaluation of a Persons level of consciousness using simple parameters such as eye opening, best verbal response and motor responses. Within each of these three parameters of the Glascow coma scale, there are a variety of responses which are arranged in scales of increasing dysfunction. Each aspect is assessed independently of the others.
Table of Contents
The three Parameters of the Glascow coma scale
- Eye opening
- Best verbal response
- Best motor response
Parameters of the Glascow coma scale
Eye Opening
- Spontaneous eye opening (4): if the eyes of the patient are noticed to open spontaneously, then a score of 4 is given. What this means is that the arousal mechanism in the reticular activating system of the brain is functioning.
- Opening to speech (3): if the eyes are closed, then you can speak to the person by calling the name or telling the person to open the eyes. Do not touch the person because it is the response from the speech that is being assessed. If there is response to a normal speaking voice, then try to increase the tone. If the patient opens eyes to speech, then a score of 3 is given.
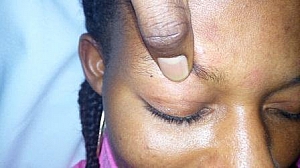
- Opening eyes to pain (2): Physical stimulation, usually in the form of pressure on the fingernail bed using a pencil or pen is applied. Another way of ensuring physical pain is stimulated is by using the knuckles of the index finger to rub on the sternum. It is important that when different medical personnel are doing this, they should all use the same method of applying physical stimulation to ensure consistent, accurate findings. However, care must be taken not to inflict injury on the patient especially that of the sternum.
- No eye opening (1): If no response is demonstrated in either eye to increased painful stimuli, there is depression of the arousal system.
- Sometimes, the patient may be sufficiently alert to respond by opening the eyes, but is restricted by swelling of the eyelids. If the eyelids are swollen and prevents the patient from opening, then C is recorded.
Scores of 3 and 4 in eye opening suggest that the cerebral cortex is processing information, even though this is also seen in the vegetative state. A score of 2 shows that lower levels of brain is functioning.
Best verbal response
The patients ability to speak and to understand the languages spoken are determined. If the patient is intubated (has a tube used for breathing) or has a tracheostomy (a surgical opening on the neck made to aid respiration), verbal response cannot be observed and T is recorded. Speech is first used to stimulate a verbal response by asking the patient simple, direct questions such as: is this your wife (if the wife is there)? Where are you? If there is no response, a light touch is used or, if necessary, painful physical stimulation. Patient responses are rated as being:
- Oriented (5): if able to respond as to who he or she is, where he or she is and give the year, month and day. You may be surprised that some may not even know the name of their husband, wife or theirs. If oriented, a score of 5 is given.
- Confused (4): if not fully oriented to time, place and person, then 4 is recorded.
- Inappropriate (3): if the patient utters words in a disorganized way, swears or does not engage in meaningful conversion, then 3 is given.
- Incomprehensible (2): when responses are limited to moaning, groaning or mumbling sounds with no recognizable words; give a score of 2.
- No response (1): when no sounds are made in response to noxious stimuli, a score of 1 is recorded.
Best motor response
The best motor response of the Glascow coma scale in either arm is usually observed by asking the patient to raise the arms forwards for about 10 seconds. The ratings in order of decreasing levels of function include:
- Obeys command (6): when the patient understands verbal, written instructions or gestures and performs the requested movement, give a score of 6.
- Localization to pain (5): this occurs when there is no response to command. A painful stimulus is then applied such as pressure on the patients fingernail bed or stimulation to an area of the head or trunk or rubbing of the knuckle of the index finger on the sternum. The patient moves a limb in an attempt to locate and remove the stimulus. In this, give a GCS score of 5.
- Flexion withdrawal to pain (4): occurs when the arm bends at the elbow in response to fingernail bed pressure or other local stimulation. Leg flexion is not a reliable gauge because with brain death, a spinal reflex may be present, causing the legs to flex in response to localized pain.
- Abnormal flexion – Decorticate (3): This occurs when a painful stimulus is applied and the arms flexes at the elbow and pronates, making a fist. If the patients arms move toward their chest, their fingers and wrists flex on their chest and they point their toes, then they are said to have decorticate posturing and a score of 3 is recorded. Decorticate posture shows there is head injury and some patients may present with this posture even before initiation of the painful stimuli.
- Abnormal extension to pain Decerebrate posture (2): occurs when the elbow straightens and the arm abducts (usually with internal rotation) in response to localized pain applied to the fingernail bed. If one arm and the other extends, the best response is recorded. If the patients arms and legs extend, their wrists rotate away from their body and they point their toes, then they are said to have decerebrate posturing and receive a score of 2. Decerebrate posture shows the presence of head injury too.
- No response (1): is recorded when no detectable movement or change in the tone of the limbs is observed in response to repeated and varied stimuli.
A score of 3 in motor responses indicates that the lesion is originating in the internal capsule or the cerebral hemispheres and is caused by disinhibition through the removal of corticospinal pathways above the midbrain. Also, a motor response score of 2 describes a midbrain to upper pontine damage and is attributed to the disinhibition of vestibulospinal tract and pontine reticular formation by removing inhibition of medullary reticular formation transection at intercollicular level between vestibular and red nuclei.
GLASCOW COMA SCALE |
|||
| Parameters | Responses | Scores | Special Conditions |
| Eye Opening | Spontaneously | 4 | Eye closed due to swelling = C |
| To Speech | 3 | ||
| To Pain | 2 | ||
| None | 1 | ||
| Best Verbal | Oriented | 5 | Endotracheal tube or Tracheostomy = T |
| Confused | 4 | ||
| Inappropriate | 3 | ||
| Incomprehensible | 2 | ||
| None | 1 | ||
| Best Motor | Obeys commands | 6 | Record the best arm response |
| Localizes to pain | 5 | ||
| Flexion/Withdrawal to pain | 4 | ||
| Abnormal Flexion (Decorticate) | 3 | ||
| Abnormal Extension (Decerebrate) | 2 | ||
| None | 1 | ||
Interpretation of the GCS scores
- GCS score of 15 is normal
- A GCS Score of 13 or higher correlates with a mild brain injury
- A GCS score of 9 to 12 is a moderate injury
- A GCS score of 8 or less is a severe brain injury
- There is no GCS score of Zero (0) even in a death patient. A death patient has a score of 3
- GCS score should be properly recorded for interpretation by taking note of each parameter such as: GCS score of 11 with Eye opening of 3, Verbal response of 4 and Motor response of 4 (that is: E3, V4, M4). The time taken should be specified to aid in monitoring to know if the patients condition is improving or worsening.
Assessment of pupil responses and limb movements provides information and assists in localizing lesions; for example, if the pupil starts to dilate, pressure on the third cranial nerve is present, and neigbouring parasympathetic fibres which control pupillary constriction are affected. This may indicate coning or herniation of brain tissue through the tentorial hiatus.
Special conditions in evaluation of GCS
- Patients who are intubated are unable to speak, and their verbal score cannot be assessed. They are evaluated only based on eye opening and motor score, and the suffix T is added to their score to indicate intubation. It therefore means that the maximum GCS score that can be recorded as would be 10T and the minimum score is 2T for such patients.
- The initial score should be assigned six hours after Head Trauma had been sustained in order to avoid overestimation of brain damage produced by transient factors, such as hypoxia, hypotension or alcohol intoxication.
- The GCS use in the assessment of the acutely poisoned patient should not be recommended. For example, after an ingestion of gamma hydroxybutyrate, many patients will not require intubation even with a GCS score of 3 if adequate ventilation and oxygenation are maintained.
The GCS attributes a score, ranging from 3 to 15. A score of 9 or less indicates Unarousable coma. For prognostication, a GCS score of less than 5 is associated with grave outcome and a score of 5 to 8 may indicate a better prognosis in a child than an adult. In Traumatic Brain injury, a GCS below 5/15 at 24 hours implies severe injury; 50% of such patients die or remain in a persistent vegetative or minimal conscious state. However, prolonged coma of up to several weeks is occasionally followed by good recovery.
Sites of physical stimulation of pain while using the GCS
- Fingertip pressure
- Trapezius pinch
- Supraorbital notch
- Sternal rub: this should be done lightly as it can cause injury on the sternum due to the thin skin on the sternum
Disease conditions in which the GCS can be used
- Vascular injuries
- Infections
- Metabolic disorders such as hepatic or renal failure, hypoglycemia, diabetic ketosis
- Almost all patients
Advantages of using the Glascow coma scale
- It is simple and can be used by Doctors, Nurses and Medical students.
- It aids in clinical decisions, such as when to intubation a patient (for total GCS score 8 or motor score of 4)
- It aids in monitoring of intracranial pressure (ICP) (for total GCS score of 13 or total GCS scores 14 or 15 with evidence of Head trauma )
- It aids in admission of patients to Intensive Care Unit (ICU)
Limitations to use of the GCS
- Cannot be used in Paediatric patients such as newborns (Apgar score is used) and children less than 4 years (Blantyre score and AVPU score are used)
- Patients on Alcohol will mask the true nature of injury to the brain
- Patients with tracheostomy
- Patients with dysphasia limits assessment of Verbal response
- Failure to incorporate brainstem reflexes is a major limitation to assessing the brain functions
- The GCS does not incorporate the size and reactivity to light of patients pupils. This would be certainly helpful, since a dilated pupil or unequal pupils not reacting to light suggest temporal lobe herniation
There are several ways to assess the conscious state of a patient (both adults and children) aside using the GCS. But each has its limitations and uniqueness. However, the Glascow coma scale is widely accepted. These alternatives to GCS include:
- AVPU score
- Blantyre score which are used in paediatric patients.
- Reaction Level Scale (RLS)
- Innsbruck Coma Scale (ICS)
- Edinburgh-2 Coma Scale (E2CS)
- Advanced Trauma Life Support
- AVPU (Alert, Verbal, Painful stimuli, Unresponsive) scale
- ACDU (Alert, Confused, Drowsy, Unresponsive) scale