Table of Contents
What is a Tracheostomy?
A Tracheostomy is an artificial opening made on the anterior part of the neck in which the upper part of the Trachea communicates with the outside air and the opening is maintained by a Tracheostomy Tube for the purpose of relieving airway obstruction or protecting the airway in certain medical conditions. It is often confused with Tracheotomy as some people used both to refer to the same thing; however, there is a slight difference medically. The difference between a Tracheostomy vs Tracheotomy is that, one is the process of creating just a hole on the trachea while the other is addition of tube to the created hole. Tracheotomy is the surgical creation of a hole on the trachea while Tracheostomy is the insertion of a Tube to the created wound. Tracheostomy may be done as an Emergency or as an Elective procedure.
Tracheostomy Indications
Tracheostomy could be done for many reasons. There are reasons for Tracheostomy in Children and also in Adults.
Tracheostomy Indications in Children
- Airway immaturity: especially in premature babies. Their respiratory structures are not yet mature, so the need to be temporarily supported until they become mature. This immaturity could be as a result of laryngomalacia and tracheomalacia (that is, the softening of the Larynx and Trachea respectively).
- Obstructing congenital anomalies: abnormalities from birth that occurred during birth or even when the baby is still in the womb such as vocal cord paralysis following closure of the patent ductus arteriosus in children with such heart defects (heart problems) or may be caused by injury during birth. Children with choanal atresia and Pierre Robin syndrome also require Tracheostomy. Congenitally stenotic airway or tracheal agenesis are special cases of Tracheostomy
- Acquired obstructions: this could be caused swallowing of foreign bodies; very common in children
- Tumors: this could be due to malignant (cancer) or benign tumors
- Trauma affecting the airway and causing inability to breathe properly
Indications for Tracheostomy in Adults
- Neuromuscular failure
- Chronic aspiration
- Laryngeal diphtheria
- Subglottic stenosis
- Severe Faciomaxillary injuries
- Chronic respiratory failure
- Sleep apnea or neuromotor problems resulting in poor airway maintenance requires a tracheostomy to be done
- Tracheostomy should be done following a major surgery that requires long term respiratory support.
- Repair of laryngotracheo-esophageal cleft
- Tracheostomy should be done in the management of tumors such as cervical teratoma or sarcoma in infancy.
- To reduce the anatomical respiratory dead space and so improve respiratory function in chest injuries, severe pulmonary disease in which tidal volume is reduced by ineffective respiratory effort such as fulminating bronchopneumonia, emphysema
- As a preliminary to total laryngectomy
- As an elective procedure to provide a route for anesthesia away from the field of surgery
Tracheostomy Procedure
- The patient will lie on the back (supine) on the operating table
- The anesthesiologist or anesthetist ensure to keep the airway patent and keeps control of it
- In Unconscious patients or in a case of Emergency Tracheostomy, no anesthesia is used;
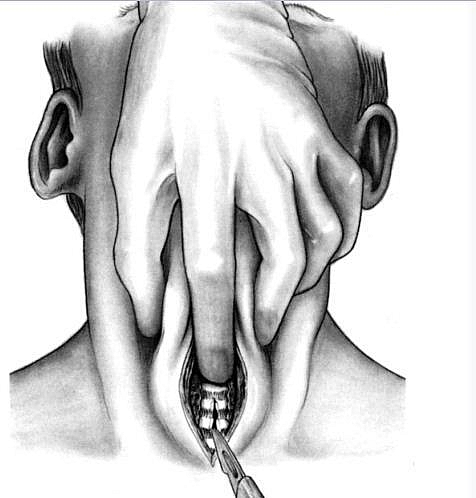
- The neck of the patient is extended properly to allow complete access to the neck. A roll can be used to enable proper positioning.
- Insertion of a bronchoscope in the trachea helps when performing tracheostomy in young children.
- An Incision is created in the lower neck crease, about the width of one finger above the jugular notch. A transverse incision is preferable and the aim is to get to the Trachea.
- When the Trachea is visualized, the proposed tracheostomy cannula should be selected, opened and its outer diameter visually checked against the exposed trachea to judge the correctness of its size.
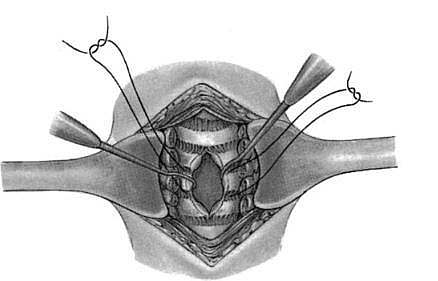
- In children, a suture of about 4/0 monofilament non-absorbable suture or its equivalent in adults is placed on either side of the midline scored anterior trachea. With each suture incorporating one or two tracheal rings. These sutures are used to hold the Tracheostomy tube in place.
Types of tracheostomy Tubes
- Metallic or latex Tracheostomy Tubes
- Cuffed or non-cuffed Tracheostomy Tubes
Types of Tracheostomy
- Elective Tracheostomy
- Emergency Tracheostomy
- Mini Tracheostomy
- High, Mid and Low Tracheostomy
- Temporary tracheostomy or Permanent
Tracheostomy could also be classified as High tracheostomy, Mid or Low Tracheostomy. It is usually done at the 2nd and 3rd tracheal rings behind the isthmus (Mid Tracheostomy). A high tracheostomy is one that is above the isthmus while a low tracheostomy is below the isthmus. A High tracheostomy is done for subglottic edema, infection or stenosis. A Low tracheostomy is indicated for injury to highly placed large vessels of the neck.
Elective Tracheostomy
The advantage of an elective tracheostomy procedure is that there is complete airway control at all times, unhurried dissection and careful placement of an appropriate Tracheostomy tube which ensures less complications. A general anesthesia is used.
Emergency Tracheostomy
This type of tracheostomy procedure is lifesaving and it is done within 2 to 4 minutes; however, the chances of complications are high. The aim is to save the life of the patient and hence you may not have the luxury of time to ensure adequate preparation.
Mini tracheostomy (Cricothyroidotomy)
Mini tracheostomy tubes measure about 3.5mm to 4 mm in diameter and are cuffless tubes usually inserted via the cricothyroid membrane. This type ofTracheostomy procedure is normally carried out with local anesthesia. There are usually two methods of performing the Mini tracheostomy (Cricothyroidotomy) which may be by the Seldinger technique or the direct trochar method. Minitracheostomy advantage allows the suctioning of secretions from the lungs without the need for formal endotracheal intubation or main tracheostomy.
Permanent Tracheostomy
This is done when the airway is permanently damaged following trauma, bilateral abductor paralysis, laryngeal stenosis or in a malignancy affecting the airway. All other types are temporary if the tubes are to be removed in a later date.
Steps and Procedure for Tracheostomy After Care
- The patient should have a bell at the bedside for summoning a nurse
- There should be a pen and a paper to enable the patient communicate as there is temporary loss of voice after Tracheostomy
- A sterile tracheal dilator, cannulas and introducers, retractors, dressings and suction tube should be available always for prompt suction in an emergency
- Suction is carried out as often as necessary at least every 2-4hrs on the first day
- The inner tube is removed and cleaned in Sodium bicarbonate Na2CO3 every 4hrs
- The air entering the trachea must be humidified by using a steam tent as the nasopharynx which normally humidifies it has been bypassed
- If Intermittent Positive Pressure Ventilation (IPPV) is used, the air must be warmed and humidified and delivered at the correct rate and pressure
- Tenacious secretions is soften with normal saline via a fine catheter
- The tube is removed when the indication for which the tracheostomy was done no longer exists, i.e. when the patient can breathe when the Tracheostomy is occluded
Tracheostomy Complications
- Tracheostomy tube displacement
- Pneumothorax (air collection in the pleural space of the lungs)
- Severe hemorrhage (bleeding following injury caused by Tracheostomy tubes especially the metallic Tracheostomy tubes)
- Wound infection: this is common and requires proper Tracheostomy care.
- Formation of crusts in the trachea or bronchi that could cause respiratory difficulty
- Surgical emphysema in the neck
- Mediasternal emphysema
- Fistula formation
- Difficulty in swallowing
- Chest infections from aspiration of secretions
- Tracheal stenosis caused by ischemic necrosis from the tracheostomy cuff, it may occur at the stoma
- Damage to the laryngeal nerve may occur and patient may not be able to speak; there may be temporary inability to speak following a Tracheostomy surgery (but this is not a complication and should be explained to the patient before surgery).